Your immune system consists of a vast network of cells, proteins, tissues, and organs that work together to maintain an optimal environment to combat attacks from foreign microorganisms. It serves as the body’s defense system, identifying and removing foreign microbes. Understanding your immune system and the factors that can influence it is the first step in maintaining healthy immune function. If you are concerned about your immune health, visit your doctor to discuss these important questions.
1. What is the immune system, and how does it function?
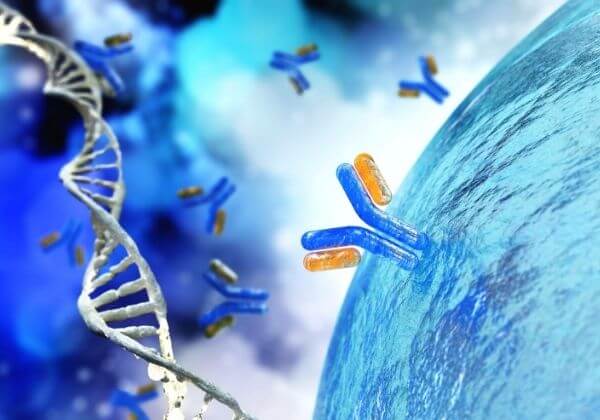
The immune system consists of specific organs, cells, and proteins that work together to protect the body. White blood cells are a variety of immune cells, and these look for invading microbes. Once identified, these cells remove or neutralize these microbes and trigger the activation of antibodies.
The thymus produces special white blood cells called T cells, while others are made in the spleen and bone marrow. Most white blood cells are present in your blood, but some are present in your tissues and the lymphatic system, which contains lymph nodes that trap microbes and fluid that processes and transports debris left from immune system activity.
Antibodies, which are also produced in the spleen, are responsible for recognizing antigens on the surface of microbes so they can be efficiently targeted for destruction. The spleen also helps with the removal of microbes from the body. The complement system is the final component of innate immunity, preventing microbes from entering the body, and adaptive immunity being brought into action by antibody activity.
Finally, with 70-80 percent of your immune system living in the digestive tract, it is essential to support proper digestive health for your body to maintain strong defenses and protection.
2. What causes poor immune health?
Several factors can impact immune system function. Primary factors that influence your immune system are genetic. Having a family member that has poor immunity can increase the risk of you having similar conditions.
There are also secondary factors or outside sources that can influence immune system function, such as:
♦ Infections
♦ Certain health conditions
♦ Limited access to nutrition
♦ Overall poor physical health
♦ Intravenous drug use
♦ High-risk sexual behavior
♦ Excessive alcohol consumption
♦ Consumption of a large number of medications

3. What are the symptoms of poor immune function?
When your immune system is not functioning properly, your overall health is at risk. Immunity can be compromised by an underlying health condition, or it can mistakenly target healthy cells for destruction. Some circumstances can cause your immune system to become overactive, as is the case with allergies.
The symptoms of poor immune function will vary across individuals, but in general, you can look for the following signs:
♦ Frequent cold and infections
♦ Overactivity or abnormally low activity of the immune system
♦ Slow-healing wounds
♦ Blood disorders
♦ Skin rashes
♦ Frequent digestive issues
♦ Fatigue
♦ Joint stiffness
♦ Numbness or tingling in your extremities
♦ Unexplained weight change
4. What are the complications of poor immune system function?
The immune system protects the body, and when these defenses are not functioning properly, there is an increased risk for complications. Most commonly, poor immune function increases the risk of unusual, recurrent, or difficult to treat infections. Symptoms of any ailments are also likely to be more severe and more difficult to overcome.
In addition to this, without a strong immune defense, the risk for the following complications also increases.
♦ Damage to heart, lungs, or nervous system
♦ Digestive function problems
♦ Slowed growth
♦ Abnormal cell growth
♦ Death from serious infection
5. How do allergies relate to immune function?
Allergies are one of the most common chronic health conditions in the world. When a harmless substance such as dust, mold, or pollen is encountered by a person who is allergic to that substance, the immune system may overreact. Antibodies are produced to attack this allergen, causing symptoms such as wheezing, itching, runny nose, and watery or itchy eyes.
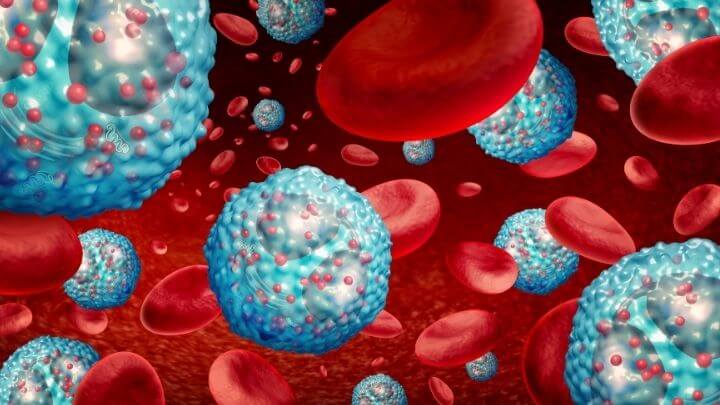
There is a strong connection between allergies and your immunity. Allergies are the result of an aberrant immune response. Chronic allergies affect your overall health in many ways, mainly through mistargeted immune system responses that can damage tissues and leave one prone to infections. Poor immune function can also amplify the immune response to allergens, causing more severe symptoms and an increased risk of developing allergies.
6. What tests are there to check immune function?
Should you seek medical attention for any of the symptoms mentioned previously, your doctor will always start with a comprehensive history followed by a physical exam. At this time, it is important to discuss your medical and family history with your doctor. Further testing may be required depending on the outcome of the physical exam. Blood tests are the most common for doctors to take a closer look at the immune cells and proteins in your blood.
Abnormal numbers of specific cells can indicate an immune system irregularity. Blood tests can also determine if your immune system responds properly and produces proteins that identify and kill foreign invaders such as bacteria or viruses (antibodies). Not having enough immune cells, having too many, or having immune cells and antibodies that are not properly working can all indicate an immune system problem.
Tests to evaluate white blood cell levels, as well as antibody levels, are the most important. A count that is higher or lower than normal can be indicative of poor immune system function. After evaluating white blood cell counts, additional testing may be required to specifically identify how the immune system is being affected so proper treatment can be advised.
7. What are my treatment options?
Treatment to support immune function will depend on the underlying cause. Antibiotics are used to treat infections, and low-dose steroids are used to address allergic responses. Immune-related symptoms such as pain and fever will be treated with medications, while decongestants are prescribed for sinus congestion, antihistamines for runny nose and sneezing, and expectorants to thin mucus in the airways.
There are also treatment options to boost immune function, including:
♦ Immunoglobulin therapy: This blood-based treatment is used to support antibody production when your immune system is unable to make antibodies necessary to defend your body.
♦ Interferon-gamma therapy: An injection is given to reduce the severity and frequency of recurrent infections. This therapy is rarely used but can be beneficial for individuals that are born with poor immune function.
8.Can a person be immune to certain conditions?
Your innate immune system offers an immediate, nonspecific reaction to an injury or microbe. The adaptive immune system takes longer to respond but launches a more targeted attack. The role of lymphocytes is key in this response. They possess memory and manufacture antibodies that attack foreign bodies. Once you have produced antibodies to a certain microbe, the risk of infection from that microbe is significantly reduced. You will already have cells that immediately recognize the foreign bodies and produce the antibodies that destroy them.
Vaccines also have a role in developing immunity by eliciting an immune response. The injection of dead or altered disease-causing microbes into healthy people allows the body to build a defense and boost the immune system. Since vaccines use an altered version of an infection, there may be mild symptoms as the body prepares its defense and builds immunity. However, they are not likely to cause illness and are beneficial in reducing the risk of serious illness.
9. What lifestyle changes can better support immune function?
Your first line of defense is always to choose a healthy lifestyle. Every part of your body, including the immune system, functions more efficiently when protected from outside harms. You can support overall health and better immune system function by adopting these healthy-living strategies:
♦ Don't smoke.
♦ Eat a balanced diet high in fruits and vegetables.
♦ Exercise regularly.
♦ Maintain a healthy weight.
♦ If you drink alcohol, drink only in moderation.
♦ Get adequate sleep.
♦ Practice good hygiene to avoid infection, such as washing your hands frequently.
♦ Try to minimize stress.
10. Are there any natural supplements that support immune function?
In addition to adopting healthy-living strategies, there are natural supplements that may improve overall immune function. In working closely with 1MD Nutrition™ researchers, more effective solutions for immune health were developed. Bu using clinically-studied, natural ingredients, the 1MD Nutrition™ immune health suite supplements can boost immune function and reduce your risk of chronic illness.
ImmunityMD® Probiotic Formula is the only immune system-supporting formula for lip, skin, and oral health that contains a proprietary blend of healing probiotics and prebiotics. This potent blend helps to support immune function by improving the gut’s ability to absorb nutrients and block toxins. With zinc to support immune cell function and l-lysine to help reduce everyday worries, ImmunityMD® is the perfect combination of probiotic strains, minerals, and amino acids to promote proper immune system function.
The increase of respiratory conditions around the world makes it essential to support and promote proper immune function. BreatheMD™ is a unique immunity and respiratory formula containing clinically effective dosages of immune-boosting vitamins, minerals, and Pelargonium sidoides. This revolutionary herb has been clinically proven to help support a healthy immune system and proper lung function, giving you total body health.

ImmunityMD® Plus couples Pelargonium sidoides with several essential immune-boosting ingredients to provide comprehensive immune system support and better strengthen the body’s defenses.
♦ L-cysteine: L-cysteine is a powerful amino acid that improves the production of glutathione, an antioxidant enzyme that helps clean and repair tissues, and thins out mucus, allowing for it to be removed from obstructing the respiratory pathways.
♦ Chromium: This element stimulates the production and activity of key white blood cells and enzymes to better support immune function and healing along the respiratory tract.
♦ Vitamin C: Vitamin C helps recycle spent vitamin E while also positively influencing the adaptive and innate immune system by strengthening epithelial tissue and improving immune cell activity to support the body’s defense.
♦ Vitamin E: This vitamin improves T-cell production, which is responsible for identifying and fighting non-host cells to ensure the immune response is adequately maintained.
♦ Vitamin D3: This vitamin is an integral part of respiratory and immune health due to its ability to support the function of immune cells, including T-cells and macrophages, that protect your body from foreign cells.
Final Thoughts
The immune system is responsible for the defense of your body and removing pathogens should they get in. Immune system function can become impaired through genetics and poor lifestyle choices, increasing the risk of chronic health conditions. It is important to support your immune system health and allow your body to have the strongest defense to reduce chronic illness risk.
The revolutionary formulas of both ImmunityMD® and BreatheMD™ are designed to support immune system healing and function. Following healthy-living strategies and regular support through 1MD Nutrition’s natural immune system health supplements will protect your health, maintain optimal immunity and enhance your overall wellbeing.
Dr. Brian Greenberg

Dr. Brian Greenberg is an immunologist, allergist, and pediatrician who received his medical degree from the University of Florida, and completed his residency and fellowship at UCLA. He has practiced medicine in Southern California for almost 25 years.