Most people experience digestive symptoms at least once a month. For many, it is a daily event that results in pain, discomfort, nausea, gassiness, bloating, or diarrhea. Few associate their symptoms with indigestion, but that is probably the most accurate term since the symptoms usually stem from poor digestion of food (“in” means lacking, as in “incomplete”).
Most of us will fail to bring it up with a medical provider, and those who do will likely receive prescriptions for pharmaceuticals that merely cover up the symptoms without solving the problem. Some will undergo invasive endoscopic procedures, which are often important to ensure the problem is not serious. But, the vast majority of us do not have a serious problem and simply need to increase digestive capacity or avoid certain foods to help relieve symptoms.
In order to help you avoid unnecessary testing and prescription medications, this article aims to teach you the questions you should ask your doctor about your symptoms. But before we begin, it is important to better understand the digestive process so that your questions are well-informed.
Understanding the Digestive Process
Digestion is an active process that costs energy. We need to use energy to gain energy. The intake of food and the breakdown of food (digestion) are the first two steps. The next step is the absorption of nutrients, which is a much more specific process than people realize. Almost all nutrients require active recognition and passage into the body.
Even water requires active transport via the sodium-glucose transporting mechanism. This discovery has led to specialized sports drinks and oral rehydration solutions that have been shown to rehydrate us better than drinking water alone. Once nutrients enter the body, they usually cycle through the liver first for filtration and processing before circulating through the rest of the body.
The ingestion of food requires proper chewing or a process called mastication. Digestion actually starts in the mouth. Chewing breaks down food and increases its surface area. This initial point of contact with food is greatly overlooked, especially in developed countries, where we have fast food, and people tend to eat quickly. Most people are guilty of forgetting to chew food properly.
If you want to maximize digestive capacity, it is important to take your time eating and chew your food properly, usually at least 20-30 chews per bite. Once a bolus of food is swallowed, it is propelled by peristalsis and gravity through the digestive tract, so posture and a relaxed setting can also make a difference in how well food is digested.
Food traverses the esophagus within seconds and then enters the stomach through the lower esophageal sphincter (LES), which also protects the esophagus from stomach acid. Unfortunately, the LES fails many times, which is a major problem. Acid taste can return up into your throat, or you may experience bloating, abdominal pain, or even a chronic cough. The most common cause of LES failure is improper digestion of food, which is one of the greatest and most hidden medical secrets in the digestive field.
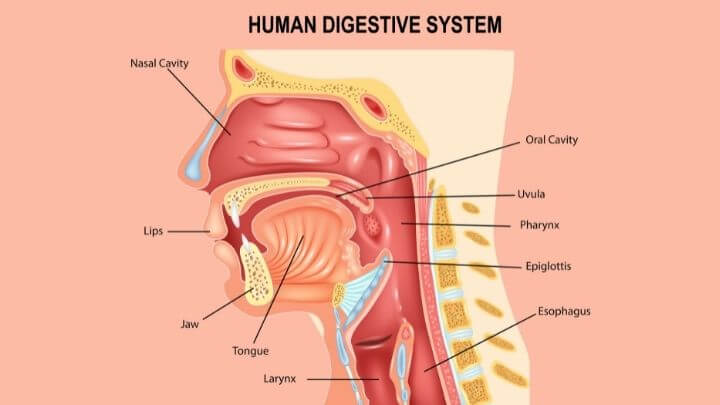
The stomach digests food with enzymes and hydrochloric acid (HCl), but it is smarter than people think. First, along with stretch receptors that tell you when you are “full,” the stomach contains chemical receptors that actually measure the content of food. The stomach knows exactly what you are eating and can even compartmentalize to digest different food differently. That way, food that is ready for release into the small intestine can be propelled forward, while food that needs more time gets pushed to the back for more digestion.
Once the food is in the small intestine, it is emulsified in bile and pancreatic juice, which neutralizes the HCl from the stomach and continues the digestive process. The small intestine is in charge of nutrient absorption, and it relies heavily on proper peristalsis to propel food forward. It takes about 6 hours to move food all the way from the stomach to the colon. The small intestine is also where most of our immune system lives. When you hear sayings like “all disease starts in the bowel,” that is the reason, and indeed a lot of aberrant immune responses are triggered by the small intestine not digesting food properly.
In summary, you do not want to ignore digestive symptoms. It is essential for you to know what to ask your doctor so that you can actually get answers, not just prescriptions or invasive and expensive tests.
Questions You Should Ask Your Doctor About Your Digestive Health
Doctor appointments are limited by time, so it is important to be prepared. To get the most benefit from your meeting, these questions can be a good place to start.
1. How do I know if a food is not being properly digested?
First, when food is not properly digested, it gets fermented by bacteria living in your gut—excess fermentation results in occasional symptoms such as gassiness, bloating, abdominal pain, and diarrhea. So your doctor should discuss your diet with you and recommend personalized dietary recommendations to eliminate or reduce potential trigger foods.
Foods that you might be having trouble with need to be substituted with food that is easier to digest. Make sure to include your family history since digestive issues commonly run in families. You also need to disclose any medical conditions that you may have that may affect your digestion, including the medications and supplements that you are taking.
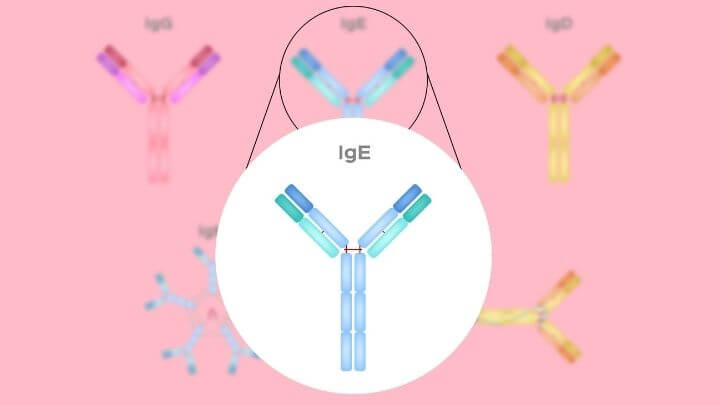
Second, if your symptoms are suggestive of an allergy, ask your doctor to do a blood test for immunoglobulin type E (IgE), which is an antibody produced by the immune system in response to an allergen. While a positive IgE test indicates that you are allergic to that food, a negative test may not be conclusive since not all allergies are mediated by IgE. Therefore, sometimes the best way to identify a food allergy (or sensitivity) is through empiric elimination of a specific food in your diet.
By far, the most common food that causes digestive issues is dairy. Cow milk products are very complex and contain bioactive molecules beyond lactose, fat, and protein. Those molecules include various oligosaccharides and peptides that are poorly digested. It is not easy to digest milk products, and many people over-consume, leading to digestive discomfort, so it is often best to eliminate dairy for a month and see if your symptoms improve or even disappear. This has worked for literally thousands of my patients.
The other common dietary triggers of both true food allergies and food intolerances (or sensitivities) include soy, wheat, eggs, peanuts, and shellfish. Sometimes tree nuts and other seafood are included in the six-food elimination diet (SFED). Studies have shown that for some digestive issues, the SFED results in a beneficial clinical response in over 80% of patients.
2. How is my diet affecting my immune system?
The majority of your immune system lives in the gut, which makes sense given that your gut is a significant source of exposure to the outside world. A lot of foreign material, both food and non-food, is introduced to the body through the gut, so the immune system has to be ready to attack and neutralize any potential threat. All of us endure potential invaders on a regular basis, so the immune system is working all the time, and balancing how much immunity you need at any one time can be a challenge.
We gain oral tolerance, a term used to describe our ability to tolerate our diet, as babies when we slowly become exposed to the world outside the womb. At first, our immune system very much resembles that of our mother, but with time, and as our guts become colonized by bacteria, our immune system becomes our own. Unfortunately, since the modern or western diet is full of unhealthy foods, our immune system can develop in a nefarious manner, leading to our immunity turning against ourselves.
Those who suffer from autoimmunity can benefit by modifying their diet to exclude foods that are poorly tolerated. Your doctor can review your dietary history and suggest specific items that should be excluded and replaced by other foods that may be less problematic. Some foods can boost immunity, such as citrus fruit, Brazil nuts, garlic, or chicken soup. What matters most is understanding the connection between poor digestion and immunity and addressing it with your doctor.
3. Do stress and fatigue affect my digestion?
It has been known for a long time that there is a very strong brain-gut connection. Only recently did we unravel the mystery of that connection. First, not only is there a cranial nerve that descends from the brain to the gut, called the vagus nerve, but we discovered that many of the neurohormones that work in the brain are actually made in the gut. In fact, about 90% of serotonin, also referred to as the happy hormone, is made in the gut.
Stress and fatigue may alter serotonin production, leading to poor mood stability and altered mental capacity. Stress can also affect motility, better known as peristalsis, where the gut moves in a snake-like motion that helps digest and push food along the small intestine and sweep away debris. Stress can alter motility and speed up or slow down this peristaltic motion. Fatigue can alter satiety signals, usually resulting in increased energy intake. So, stress and fatigue affect digestion on multiple levels.
It is important that you discuss stressful events in your life with your doctor and review your sleep pattern. Behavioral and cognitive therapy may be indicated not just for mental health but will also help your digestive system.
4. What is the best way to increase digestive capacity?
There are various medications that can relieve symptoms of digestive distress, but none of them solve the true nature of the problem. Modifying your diet to avoid problematic foods is one approach for better digestion, but to truly increase digestive capacity, your gut needs to break down food better. This involves stimulating the production of digestive enzymes and coordinating motility.
Digestive enzymes are produced naturally in the stomach and along the small intestine. Our genetic makeup determines, to a large extent, the production of digestive enzymes, but it is possible to stimulate further production. The use of probiotics, for example, has been shown to help stimulate the production of digestive enzymes. Healthy bacteria aid digestion and can help increase digestive capacity, so things that promote a healthy microflora will ultimately translate into better digestion.
Drugs that lower stomach acidity are commonly prescribed to alleviate symptoms of indigestion, but they do not help digestion. In fact, lowering stomach acidity can make things worse in the long run and increase the risk of serious complications. A better approach, as stated above, is to increase the gut’s ability to digest food rather than block acid production.
One other very easy manner to increase digestive capacity is to improve chewing. Slowing down our eating, increasing the number of chews per bite, and eating in a relaxed and stress-free environment can help digest food better. Discuss this with your doctor before asking for medications.
5. Are there natural supplements I can take to boost digestive health?
Modern medicine is often reactive rather than preventative, and most medical therapies for digestive issues merely cover up symptoms rather than correct the root cause. This is not your only option, as it is possible to solve digestive issues naturally, through dietary modification and by increasing digestive capacity. It is also possible to take natural and clinically proven supplements to assist the healing process and also prevent future complications.
First, probiotics are a great way to boost digestive health naturally and are considered incredibly safe and effective. 1MD Nutrition’s Complete Probiotics Platinum® is a proprietary blend of robust and potent probiotics strains, including L. rhamnosus GG, a well-studied and clinically suggested strain. This formulation was designed to help create a gut environment that is more conducive to a healthy microbial balance as well as stimulate host responses that support digestion and promote immune health.
Another great, naturally sourced supplement is prebiotics, which are a kind of digestive fiber that nourishes good bacteria in your gut. Prebiotics help foster a healthy microbial balance and promote specific beneficial strains of bacteria. PrebioMD® is formulated to support the bacterial strains you want, helping the gut establish colonization resistance, which is the unique property of being colonized with a healthy and robust microbiota that resists invasion by harmful bacteria.

In addition to probiotics, which up-regulate the expression of digestive enzymes, and prebiotics, which foster a healthy microbial balance in the gut, another naturally sourced supplement that aids digestion is EnzymeMD®. This formulation supports digestive capacity directly and immediately by helping break down food on contact in the stomach. With eight potent, plant-based digestive enzymes combined with an essential probiotic called S. boulardii, EnzymeMD® is a great way to achieve relief to many digestive symptoms and support overall digestive health.
Final Thoughts
The digestive system is essential to immune function, mental health, and overall well-being. Certain dietary and lifestyle choices can compromise digestive function and increase the risk of chronic health conditions. The above 5 questions can help prepare you for discussing your digestive health with your doctor and potentially avoid invasive medical tests and medications.
Support your gut health with natural and clinically effective supplements that promote digestive capacity and support a healthier microbial environment. 1MD Nutrition’s Complete Probiotics Platinum® combined with PrebioMD® and EnzymeMD® can provide you with the solution you need to ensure optimal digestive health and better overall well-being.
Dr. David Kahana
![]()
Dr. David Kahana is board certified in Pediatrics and Gastroenterology through the American Board of Pediatrics (ABP), as well as Medical Nutrition through the National Board of Physician Nutrition Specialists.