One the leading causes of death in both men and women in the United States, which is 655,000 people each year, is poor heart health. The heart functions to collect blood from the body, send it to the lungs to receive oxygen, and then pump that oxygenated blood to the remainder of the body.
A healthy lifestyle is critical for the heart to function properly. By speaking with your doctor about heart health, you can learn the best ways to promote optimal heart function and reduce your risks of more serious problems. Below are the top questions you should be discussing with your doctor.
1. What are my risk factors for heart problems?
There are several risk factors that can cause poor heart health, many of which we cannot control.
♦ Age: While heart health can be impacted at any age, the risks of serious heart problems increase as you get older. The most common age-related change is stiffness and hardening of the arteries.
♦ Genetics: Genes control aspects of the cardiovascular system, including the strength of arterial walls and how heart cells communicate. There are some heart conditions that can be passed down through families.
♦ Gender: Poor heart health and serious heart conditions are more common in men than women, particularly before menopause.
However, there are also several risk factors that we can control to help promote healthier heart function. Almost half of all Americans have at least 1 of the top 3 key risk factors of poor heart health:
♦ High cholesterol: Elevated LDL cholesterol levels increase the risk of plaque formation in the arteries, limiting blood flow.
♦ High blood pressure: The strain of high blood pressure through the arteries can increase the risk of damage and block blood flow to the heart.
♦ Smoking: Chemicals in tobacco can cause blood to thicken and clot, which can disrupt circulation.
Additional factors that can increase your risk include:
♦ Blood glucose levels: Over time, high blood sugar can damage blood vessels and the nerves that control your heart.
♦ Weight: Excess weight can increase blood glucose levels, raise blood pressure, and is often associated with an unhealthy diet, which is another risk factor.
♦ Unhealthy diet choices: Poor food choices include saturated fats, sugars, and processed foods. These can contribute to elevated cholesterol and blood sugar levels, which are linked to poor heart health.
♦ Lack of exercise: Regular exercise is important for healthy cardiovascular function. Inactivity or a sedentary lifestyle can lead to fatty deposits that can clog arteries.
2. What are the symptoms of poor heart health?
Symptoms may not always be present, and those reporting symptoms can experience varying degrees of severity. The most common symptoms to look for include:
♦ Chest discomfort or tightness
♦ Shortness of breath when you exert yourself or when you lie down
♦ Fatigue and weakness
♦ Swelling in your legs, ankles, and feet
♦ Rapid or irregular heartbeat
♦ Reduced ability to exercise
♦ Persistent cough or wheezing
♦ Increased need to urinate at night
♦ Swelling of your abdomen
♦ Very rapid weight gain from fluid retention
♦ Lack of appetite and nausea

3. Are men or women more at risk for heart problems?
As mentioned earlier, men have a greater risk of developing heart issues than women. Reduced testosterone can be a reason for this. However, heart problems are the leading cause of death in both men and women.
Men tend to develop heart conditions at younger ages than women, but after menopause, their risk comes closer to that of men. Reduced estrogen levels, which occur with menopause, are believed to play a role in arterial hardening. Before menopause, estrogen is believed to have a beneficial effect on the lining of the arteries.
Women are less likely than men to have the typical symptoms of poor heart health. While they may have the typical chest pressure and shortness of breath with radiation of pain to the neck and jaw and left arm, they may also present instead with back pain, fatigue, abdominal pain, nausea, or vomiting.
4. How does my family history affect my heart health?
There is a reason that doctors ask about your family health history. With regards to heart health, genetics and family history play an important role. Family health history provides information about both genetics and the environment. You cannot change genetics, but you can certainly change your lifestyle and environment to reduce possible risks.
Several genes have been identified which are associated with an increased risk of poor heart health. In addition, there are some conditions affecting blood pressure and cholesterol levels that can be passed through genes. However, it is possible that these conditions may cluster in families due to family members sharing the same unhealthy habits.
5. Are blood sugar levels related to heart health?
Blood sugar levels impact heart health and function. Elevated blood sugar levels can damage blood vessels, leading to the accumulation of plaque within the arteries. This can affect blood flow and ultimately can lead to a clot, which can be life-threatening. In addition, impaired blood vessels increase the risk of high blood pressure, which can further compound the problem. High blood sugar can also damage the nerves that control your heart.
Heart conditions are more likely to develop at a younger age in those that do not properly manage their blood glucose. The longer you have uncontrolled blood sugar, the greater your risk is for serious heart problems. You can reduce your risk by properly maintaining blood sugar through diet and lifestyle choices and monitoring your blood pressure and cholesterol.
6. Is there a link between cholesterol and poor heart health?
High cholesterol is one of the top risk factors for poor heart health. LDL, low-density lipoprotein, is known as the “bad cholesterol,” which transports cholesterol from the liver to cells. HDL, high-density lipoprotein, is known as the “good cholesterol,” which functions in the opposite manner of LDL. HDL cholesterol carries cholesterol from the cells of the body back to the liver, where it can be removed from the body.
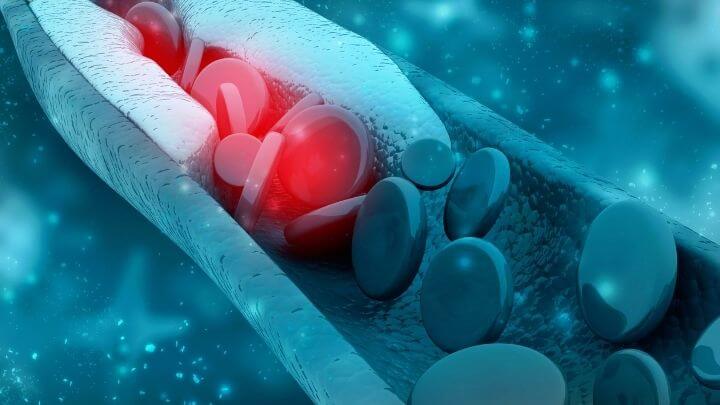
Cholesterol is not always a bad thing, as the body needs it to function. What most people do not realize is that our bodies make more than enough. Diets high in trans fats, saturated fats, and sugars can increase the levels of bad cholesterol in your body. As levels of LDL increase, so does the risk of fatty deposits that can clog arteries and interfere with proper circulation.
7. Is my level of stress increasing my risk of heart complications?
Stress can take its toll on your entire body and can be acute or chronic. Acute stress, when intense enough, can cause serious heart problems in a person that has had no previous conditions. Chronic stress may cause continued wear to the heart and blood vessels through aberrant immune responses mistakenly attacking them.
In addition to the physiological impacts of stress, it can also affect your behavior. Common lifestyle changes from chronic stress include not exercising and eating unhealthy foods. These unhealthy lifestyle choices contribute to high blood pressure and cholesterol levels, which increase the risk for heart complications.
8. Is being overweight affecting my heart health?
Being overweight can take its toll on the entire body, and the heart is no exception. An unhealthy weight puts strain on the heart but not in the physical way it impacts your joints, bones, and muscles. Carrying additional weight increases blood glucose levels, which in turn will negatively impact heart health.
There is also a link between extra weight and elevated cholesterol levels and blood pressure. One of the most effective ways to reduce your risks and encourage healthier heart function is through losing weight, exercising, and eating a balanced diet.
9. Can lifestyle changes help my heart health?
In addition to appropriate medications, changes to your lifestyle can positively impact your heart health. A study analyzing over 55,000 people showed those with favorable lifestyle habits such as not smoking, losing weight, engaging in regular physical activity, and eating a healthy diet lowered their risk of heart problems by nearly 50%.
A diet pattern high in fruits, vegetables, and whole grains and low in processed foods, animal fats, and added sugars is associated with a reduced risk of heart problems. Regular exercise is also potent in reducing your risk. If you are a smoker, quitting smoking is the most essential thing that you can do to start taking care of your heart.
10. Are there natural ways to support heart health?
The diet and lifestyle modifications suggested above are a great way to support optimal heart function and reduce the risk of serious complications. In addition to these changes, there are natural ingredients that have been clinically studied for the benefits they have for heart health. These ingredients can be found in 1MD Nutrition’s heart health suite supplements.

CholestMD®️ includes ingredients that improve cholesterol levels, which in turn can promote healthier heart function.
♦ Bergavit®️: Bergavit®️ is a patented, clinically studied, standardized extract containing the main active flavonoids of bergamot juice. This potent ingredient works to support healthy blood lipid levels to promote cardiovascular health.
♦ Niacin: Cholesterol and triglycerides are the two common blood fats that can damage your arteries and heart. Niacin lowers triglyceride levels by inhibiting the enzyme involved in the synthesis of triglycerides, reducing the risk of plaque formation.
♦ Olive leaf: Olive Leaf Extract provides naturally occurring polyphenols that support healthy lipid levels and blood circulation.
♦ Garlic bulb extract: This extract contains naturally occurring allicin, which supports metabolic function and aids in stabilizing blood lipid levels.
GlucoseMD®️ can help maintain healthy blood sugar levels and aid management of glucose uptake with clinically studied ingredients, including:
♦ Cinsulin®️: This patented cassia cinnamon extract has been shown in clinical studies to promote proper sugar metabolism, which helps maintain healthy blood glucose levels.
♦ Berberine bark: This extract is clinically shown to help support normal blood sugar levels and enhance sugar uptake from the blood into the muscles.
♦ Chromium: This common element works to support the activity of pancreatic cells that aids the body’s absorption of glucose.
Final Thoughts
With poor heart health being a leading cause of death, taking care of your heart has never been more important. Understanding the risks and what you can do to reduce them is essential to promoting heart health. Preventative care through lifestyle changes is the most potent step you can take.
A daily routine consisting of a balanced diet, regular exercise, and dietary supplement support can help you care for your heart. The broad-spectrum formula of CholestMD®️ or the targeted blood sugar support of GlucoseMD®️ supports healthy circulation, metabolic function, and overall cardiovascular health.
Dr. Heather Shenkman
Dr. Heather Shenkman is a board certified interventional cardiologist. She completed a six year program at Albany Medical College, graduating at the age of 23. She completed her residency at Henry Ford Hospital, cardiology fellowship at the University of Rochester, and interventional cardiology fellowship at the esteemed Tufts Medical Center in Boston.