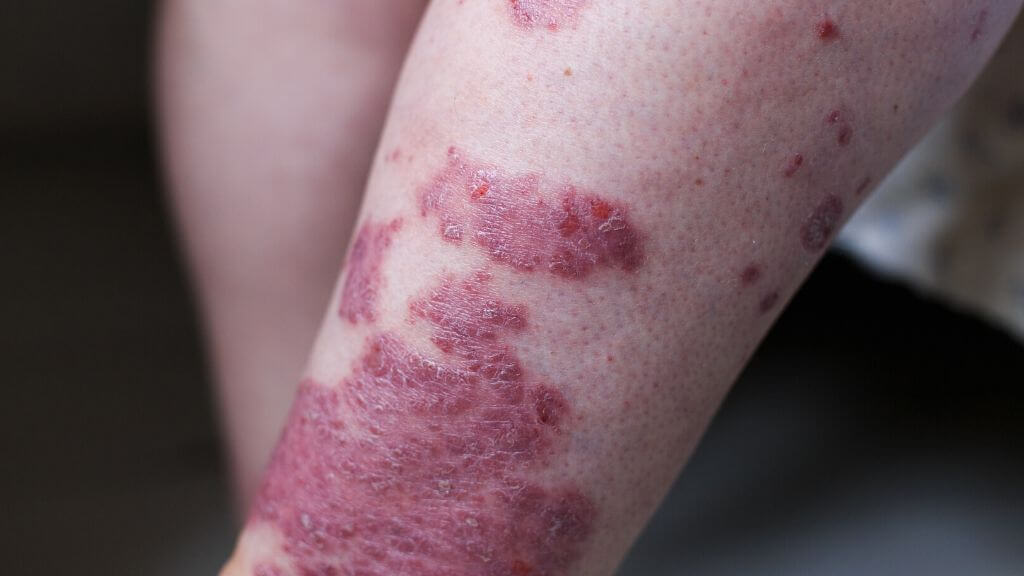
Psoriatic arthritis is a disease consisting of both psoriasis (a skin inflammation condition) and swollen and painful joints. Psoriasis typically causes itching and scaly patches to appear on the skin while arthritis attacks your joints, leaving them inflamed and painful to move.
The disease varies in its effects from person to person and can be mild or very severe. It occurs in both men and women and typically shows up between the ages of 30 and 50.
What Causes Psoriatic Arthritis?
Psoriatic arthritis is caused by your immune system attacking your joints, and the reason for these attacks is unknown. Studies indicate that genetics, as well as environmental factors, contribute to these attacks and flare-ups.
Psoriatic arthritis also runs in families, and you are 40 percent more likely to have it if a relative does too. Conditions and situations that can trigger flare-ups include stress, cold weather, smoking, excessive alcohol consumption, excess weight, infections, and injuries like sunburn or cuts.
Psoriatic Arthritis Symptoms
The symptoms for psoriatic arthritis vary for each individual, ranging from mild to severe, and sometimes they can go into remission. The general symptoms of psoriatic arthritis include:
♦ Swollen tender joints
♦ Swollen fingers and toes
♦ Morning stiffness
♦ Flaky scalp
♦ Scaly patches of skin that gets worse when joint pain flares up
♦ Fatigue
♦ Eye redness
♦ Nails separating from the nail bed
♦ Painful muscles
Psoriatic Arthritis Diagnosis
Your doctor needs to rule out other causes before giving a diagnosis of psoriatic arthritis. This is done with imaging and blood tests.
A low red blood cell count is common with psoriatic arthritis. Rheumatoid factor is also used to make sure you do not have rheumatoid arthritis, and your joint fluids are checked for uric crystals to rule out gout. X-rays will look for bone damage not caused by psoriatic arthritis.
Treatment for Psoriatic Arthritis
The goal of psoriatic arthritis treatment is to improve symptoms like skin rash and joint inflammation.
Typical treatment plans include one or a combination of the following:
♦ NSAIDs: These anti-inflammatory medications control inflammation and reduce joint pain.
♦ DMARDs: Disease-modifying antirheumatic drugs are given to reduce inflammation and prevent point damage. They can be given orally or injected and help slow the progression of psoriatic arthritis.
♦ Biologics: Synthetic drugs produced by living organisms that directly target the part of your immune system responsible for inflammation.
♦ Steroids: These drugs lower inflammation, especially when injected directly into the affected joints.
♦ Topical treatments: Gels, creams, and ointments are prescribed to help relieve itching for psoriatic arthritis rash.
♦ Light therapy: Medication followed by bright light exposure is used to treat psoriasis skin rashes.
Psoriatic Arthritis Diet
There is no diet that will cure psoriatic arthritis, but there are diets that can reduce inflammation and ease symptoms. The foods you want to include more of are:
♦ Omega-3 fatty acids: Foods containing DHA and EPA will deliver powerful anti-inflammatory compounds to reduce inflammation and joint pain. Eat more foods like fatty fish, olive oil, nuts, and avocados.
♦ Antioxidants: Oxidative stress has been found to be strongly linked to psoriatic arthritis pains and flare-ups, so foods that are high in antioxidants can prevent this. Eat more berries, leafy greens, nuts, and dark chocolate.
♦ Whole grains: Weight control is critical for those with psoriatic arthritis, and high-fiber foods are the solution. Foods like quinoa, corn, oats, and brown rice will slow digestion, maintain blood glucose levels and weight, and reduce psoriatic arthritis flare-ups.
There are also foods you want to avoid, such as red meat or processed meats as these trigger inflammation and contribute to obesity. Avoiding or limiting dairy is also important, as lactose is a common allergy that can trigger the immune system and inflammatory responses.
Processed foods that are high in fats and sugar also need to be avoided. This will help prevent obesity, high cholesterol, and elevated blood glucose levels, all of which cause inflammation.
Psoriatic Arthritis Natural Treatment
Dietary changes and medical treatments from your doctor work wonders, and there are also natural treatment options that work for psoriatic arthritis relief.
Supplements
Turmeric is a powerful anti-inflammatory spice that can reduce flare-ups and joint pain. Vitamin D is important for bone strength and health, and when deficient, you are more at risk for developing psoriatic arthritis, so try a supplement for preventative measures.
Probiotics also help by supporting the health of your gut bacteria, which have a strong influence over your immune system and inflammatory activity.
Hot and Cold Therapy
Heating pads can help to loosen stiff joints and relax muscles. You can also use heating blankets or soak in a hot bath. Cold packs reduce swelling and are best used during the day, then switching to heat therapy at night.

Because getting adequate sleep is important to reducing inflammation, these therapies combined will help you get the sleep you need.
Exercise
Regular movement will help prevent stiffness and improve muscle strength as well as maintain bone density. It also boosts your mood, reduces fatigue, and can help you to lose weight and reduce pressure on your joints.
Variations of Psoriatic Arthritis
There are five different types of psoriatic arthritis.
Symmetric PsA: This affects the same joints on both sides of the body and tends to be milder and less likely to cause joint deformations. This type, however, can be disabling.
Asymmetric PsA: Only joints or a joint on one side of your body is affected, and they may feel sore and turn red in color. This type is generally considered to be mild.
Distal interphalangeal predominant PsA: The joints closest to your nails are affected if you’re diagnosed with this type. These distal joints become swollen, but this is very rare only occurring in about 10 percent of the cases.
Spondylitis PsA: Your spine from your neck to your lower back can be affected by this type and movement is very painful. In many cases, the hands, arms, feet, and legs are also affected.
Psoriatic arthritis mutilans: This is a very severe form of RA characterized by resorption of bones and the collapse of soft tissue.

Psoriatic Arthritis Statistics
♦ More than 8 million Americans currently have psoriasis.
♦ Between 10 and 30 percent of those with psoriasis develop psoriatic arthritis.
♦ The economic burden of psoriatic arthritis is huge, as it causes negative physical, psychiatric, and social consequences.
♦ One in three people will have a relative that also has the disease.
♦ If one parent has this condition, the child has a 10 percent chance of acquiring it, but if both parents have it, the risk increases to 50 percent.
Psoriatic Arthritis and Disability
Psoriasis is the chronic skin condition associated with this disease, and for most people, it is an annoyance.
In some cases, it can form lesions and frequent infections that make it difficult to work or perform daily tasks. If the lesions make it difficult for you to move or limit the use of your hands, which is commonly called psoriatic arthritis hands, then psoriatic arthritis can be considered a disability. Lesions can also appear on your feet, making it difficult to walk.
Psoriatic Arthritis and Children
Children can get psoriatic arthritis, and the symptoms will vary from mild to severe. They typically experience:
♦ Swollen joints
♦ Inflammation of the eyes
♦ Arthritis in the lower back or spine
♦ Morning stiffness
♦ Peeling of the nails
♦ Swollen fingers and/or toes
What Is the Long-Term Outlook?
The outlook for individuals with psoriatic arthritis will vary because symptoms vary so widely for everyone. With some having mild symptoms and others having debilitating pain and quality of life disruptions, there is no way to provide an accurate outlook for all.
The more severe your condition is, the more difficult it will be for you to get around. Developing a treatment program to address and treat your symptoms is the only way to prevent psoriatic arthritis from debilitating you.