Your heart functions to provide oxygen and nutrients to the organs and tissues of your body. If your heart is not functioning properly, your health will suffer. Age-related changes can increase your risks, so being proactive about heart health is important. You cannot stop the aging process, but you can make lifestyle changes to better support heart function and overall health.
As we age, the heart walls and valves thicken. As a result, the heart no longer beats as fast during physical exertion or emotional stress as it did when younger due to fatty deposits and scarring of the heart’s electrical system. Stiff arteries lead to elevated blood pressure, while a less elastic heart increases the risk of congestive heart issues.
With a proactive approach to heart health, you can reduce the risks associated with these changes. This includes making several lifestyle changes, such as eating a healthy diet and getting regular exercise. It also includes regular evaluation of your heart function to better support heart health.
Risk Factors For Poor Heart Health
Along with the natural changes caused by aging, additional risk factors can contribute to the development of serious heart conditions.
♦ Gender: Men are more likely to develop heart problems at younger ages, but after menopause, women do gradually catch up in incidence.
♦ Genetics: If you have one or more close relatives who had heart problems at a young age, you may also be prone to heart problems at a young age.
♦ Smoking: If you smoke, consider quitting because smoking increases the risk of serious problems by two to four times.
♦ Inactivity: A sedentary lifestyle significantly increases the risk of heart problems.
♦ Poor diet: A diet low in fruits and vegetables and high in sugar, processed foods, and animal fats increases the risk of heart problems.
♦ Obesity: Carrying excess weight places additional strain on the heart.

♦ Cholesterol: Elevated LDL cholesterol and triglyceride levels can damage the heart. A healthy diet and regular exercise can help lower cholesterol levels.
♦ High blood pressure: Uncontrolled elevated blood pressure greatly increases the risk of heart problems.
♦ Uncontrolled blood glucose levels: Uncontrolled blood glucose levels will increase the risk of heart problems. A healthy diet and regular exercise can help control glucose levels.
♦ Stress: Stress triggers aberrant immune responses that can damage heart cells and tissues, so managing your stress is important. It will also help you to make wiser choices for your health, including making more healthful eating choices and finding the time to exercise.
Early diagnosis of issues with heart function can lead to a more efficient treatment to prevent and resolve potentially serious complications. In addition, understanding the contributing factors of failing heart function can help you seek evaluation and treatment early.
Evaluating Heart Health
Evaluating heart function is important, especially if you have symptoms or risk factors for poor heart health. A range of conditions that can affect your heart, including:
♦ Abnormal heartbeat is when the heart beats too fast, too slow, or irregularly.
♦ Acquired or hereditary heart muscle conditions that make it difficult for the heart to pump blood around the body
♦ Blood vessel conditions happen when arteries become narrowed or blocked.
♦ Congenital issues or heart defects that you are born with
♦ Heart valve issues happen when the valves do not work properly, which disrupts blood flow.
♦ Infection caused by bacteria or viruses can be life-threatening.
Any symptoms that indicate poor heart function should not be ignored. The symptoms of poor heart health may include:
♦ Shoulder and chest aches
♦ Shortness of breath or fatigue
♦ Dizziness or lightheadedness
♦ Swollen legs and feet
♦ Persistent cough
♦ Cold sweats
♦ Sexual dysfunction
♦ Snoring and sleeping problems
These symptoms can indicate poor heart health and the need for prompt evaluation. Early identification of issues is recommended for the most effective treatment outcomes.

Understanding Heart Function Tests
Heart function tests allow your doctor to identify any functional issues with your heart as well as monitor any age-related changes that may increase your risk of poor heart health. Because poor heart health is a leading cause of premature death, it is important to identify any problems as soon as possible. The following tests are most commonly done to evaluate the health of the heart.
♦ Electrocardiogram (ECG or EKG): An electrocardiogram evaluates the electrical activity of the heart. From this, your doctor can get clues of heart rhythm disturbances or the sizes of the heart’s chambers.
♦ Chest X-rays: A chest x-ray can evaluate the lungs, the heart, and major blood vessels of the chest. The size and position of the heart can be assessed, as well as clues of possible enlargement of heart chambers.
♦ Echocardiogram: An echocardiogram is an ultrasound of the heart. This test uses sound waves to assess the size and function of the heart, the size of the chambers of the heart, the function of the valves of the heart, and the flow of blood through the heart.
♦ Coronary Angiogram: Catheters are advanced to the heart, and dye is injected directly into the arteries of the heart while moving x-ray images are obtained. This can determine the anatomy of the arteries and identify if there are significant narrowings. With this test, measurements of the pressures of the chambers of the heart and the lungs can also be obtained.
♦ Magnetic Resonance Imaging: An MRI is an imaging test that can provide detailed information about the structure and function of the heart. It can also detect subtle abnormalities in the heart muscle tissue, which can help diagnose several heart problems.
♦ CT (Computerized Tomography) of the Heart: A CT without dye can determine the amount of calcium in the arteries of the heart, which can help provide information about a person’s risk of heart problems. A CT of the heart with dye can provide information about the arteries of the heart, though not with the same detail that a coronary angiogram would provide.
♦ Transesophageal Echocardiogram (TEE): For a TEE test, the patient is sedated with medication to prevent discomfort while ultrasound pictures of the heart are taken from inside the esophagus. This provides much more detailed information than a standard echocardiogram.
Additional testing to evaluate your heart rhythm can include:
♦ Holter Monitor: A monitor worn for 24-48 hours to detect the heart rhythm and look for any abnormal rhythms.
♦ Event Monitor: A monitor for evaluating the heart’s electrical activity over a period that is typically 7-21 days.
♦ Implantable Event Recorder: Also called a loop recorder, this is a small device implanted under the skin that can detect the heart’s electrical activity over the course of up to two years. The device can be interrogated to determine what rhythms have been detected and can also be removed when it is no longer needed.
♦ Transtelephonic Pacemaker/ICD Transmission: For those with a pacemaker or defibrillator implanted in their chest, these devices can be evaluated from a patient’s own home with a device that transmits information from the pacemaker or defibrillator.
♦ Exercise Stress Testing: A patient is connected to a heart monitor and exercises on a treadmill or bicycle. The intensity of the exercise is gradually increased, and the electrical activity of the heart is evaluated as the heart is stressed by exercise.
♦ Electrophysiology Study: This is an invasive test performed at a hospital involving the insertion of catheters into the heart, where the electrical activity is evaluated from inside the heart. This test can localize the spot where particular abnormal heart rhythms are coming from.
With proper testing and evaluation, you and your doctor can plan for the most effective course of treatment and proactive care to prevent more serious problems from developing.

Treatment Options for Heart Health
Treatment depends on the underlying contributing factors of poor heart function and varies widely, including lifestyle changes, medications, surgery, stents, pacemakers, and ablation.
Medications
♦ Anticoagulants: Blood thinner medications are appropriate for conditions such as irregular heartbeat, which increase the risk of the formation of blood clots.
♦ Antiplatelet Agents and Dual Antiplatelet Therapy: Antiplatelet medication may be recommended to reduce the risk of serious heart problems. Two different antiplatelet medications are prescribed after a coronary stent is placed to open a blocked artery.
♦ ACE Inhibitors and Angiotensin II Receptor Blockers: A type of blood pressure medication, which is also used for congestive heart problems to help improve heart function.
♦ Angiotensin Receptor-Neprilysin Inhibitors: A medication beneficial for congestive conditions to help improve heart function and prolong life.
♦ Beta-Blockers: These medications can treat high blood pressure or heart-related chest pain, or congestive conditions. They are often prescribed to help relax the heart muscle and can be used for heart rhythm problems.
♦ Calcium Channel Blockers: These medications help lower blood pressure, reduce chest pain, and treat certain heart rhythm problems.
♦ Cholesterol-lowering medications: There are many types of medications that can help lower cholesterol, some of which can help reduce the risk of arterial plaque development.
♦ Diuretics: These are medications given to eliminate excess fluid in the body, which can occur with congestive issues.
♦ Vasodilators: These medications can help decrease blood pressure or help improve blood flow to the heart.
Surgical Options
♦ Ablation: This can be done by catheter or with surgery to restore normal heart rhythm. Many abnormally fast heart rhythms are triggered by areas of abnormal heart tissue, and by ablating these, scar tissue that develops can help prevent this from happening again.
♦ Pacemakers: A pacemaker is a small device that's placed under the skin in your chest to help control your heartbeat. The device generates electrical impulses to cause the heart muscle chambers to contract and pump blood to regulate the function of the electrical conduction system of the heart.
♦ Angioplasty: Angioplasty is a procedure to restore blood flow through the artery. Your doctor threads a thin tube with a tiny balloon at the end through a blood vessel to the involved site in the artery. Once the tube is in place, the doctor inflates the balloon that pushes plaque outward against the wall of the artery, widening it to restore healthy blood flow.
♦ Stents: A stent is a wire mesh tube used to prop open an artery during angioplasty. The stent stays in the artery permanently to keep the passageway open and prevent plaque formation.
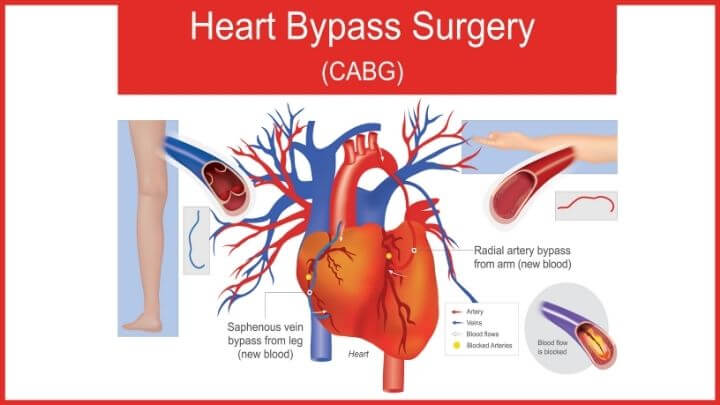
♦ Bypass surgery: The chest is cut open, and arteries from the chest wall or arm, or veins from the leg, are used to reroute blood around blockages in arteries.
Lifestyle Changes
♦ Physical activity: Doing a minimum of 150 minutes of moderately intense activity per week is recommended, or five 30-minute sessions of exercise per week.
♦ Healthy diet: Eating a plant-forward diet with plenty of fruits and vegetables, whole grains, beans, and legumes can help keep your heart healthy for years to come.
♦ Quit smoking: If you smoke, quitting smoking is the most important thing that you can do to reduce your risk of heart problems.
♦ Healthy weight: Maintaining a healthy weight through regular physical activity and a healthy diet is important, without large fluctuations in weight gain and loss.
♦ Manage blood glucose: By regulating blood glucose levels, you can reduce the risk of damage to blood vessels that can be associated with high blood glucose levels.
♦ Manage cholesterol: Maintaining healthy cholesterol levels reduces the risk of clogged arteries.
Natural Treatment To Boost Heart Function
Along with healthy living, you can also help maintain proper heart function with naturally sourced supplements. Certain natural ingredients have been identified through extensive clinical research to help support heart health. 1MD Nutrition™ includes many of these ingredients in CholestMD®️ and GlucoseMD®️, two of their physician-approved heart-healthy supplements.

CholestMD®️
♦ Bergavit® is a patented bergamot extract that has been clinically studied for its support of cardiovascular health through maintenance of healthy blood lipid levels.
♦ Niacin is an important vitamin for heart health that works to lower triglyceride levels in the blood by inhibiting the activity of an enzyme involved in triglyceride synthesis.
♦ Niacin also reduces cholesterol levels to protect the arteries from plaque formation.
♦ Olive leaf extract has been shown in clinical studies to promote healthy blood flow and blood pressure levels by helping reduce cholesterol in the blood.
GlucoseMD®️
♦ CinSulin®️, a patented cassia cinnamon extract that has been shown in clinical studies to promote proper sugar metabolism
♦ Berberine bark extract is a bioactive plant compound clinically shown to help support normal blood sugar levels and support sugar uptake from the blood into the muscles.
♦ Chromium picolinate has been shown to support the activity of pancreatic cells that work to promote the absorption of glucose to help maintain healthy blood glucose levels.
♦ Gymnema Sylvestre has been shown to support healthy fasting blood sugar levels.
Final Thoughts
Poor heart health may be the most common cause of death and disability in the world, but there is so much that you can do to keep your heart healthy. While there is clearly a role for medications, adopting a holistic approach to accompany medical care is beneficial for heart and overall health.
There is a significant benefit to having a healthy lifestyle, incorporating a balanced diet, regular exercise, stress management, and natural healing into your daily life. You can promote cardiovascular health and avoid many heart conditions from returning by taking preventative measures and promoting heart health from within.
Dr. Heather Shenkman
Dr. Heather Shenkman is a board certified interventional cardiologist. She completed a six year program at Albany Medical College, graduating at the age of 23. She completed her residency at Henry Ford Hospital, cardiology fellowship at the University of Rochester, and interventional cardiology fellowship at the esteemed Tufts Medical Center in Boston.