Mouth redness is a sign of inflammation and is also known as stomatitis. This inflammation and redness can be very painful and can cause your gums, inner lips, inner cheeks, and tongue to be sore.
Mouth redness and pain can make it difficult to eat or drink and can be disruptive to daily life as well as health. It can also be a sign of a medical condition that needs prompt treatment.
Causes of Mouth Redness
Mouth redness is a collective term for the redness on your gums, palate, inner cheeks, or tongue. The color can change to a darker red or blisters can develop. Blisters are very painful and can interfere with eating and drinking.
Inflammation of the mouth and mouth redness can be caused by trauma, but in most cases, there is an underlying condition causing the redness and pain. The most common causes are herpes simplex virus (or a cold sore) or aphthous stomatitis (a canker sore).
Herpes Simplex Virus
HSV-1 is the virus known to cause cold sores and mouth redness. It is more common among younger children, but once contracted, the virus remains with you for life.
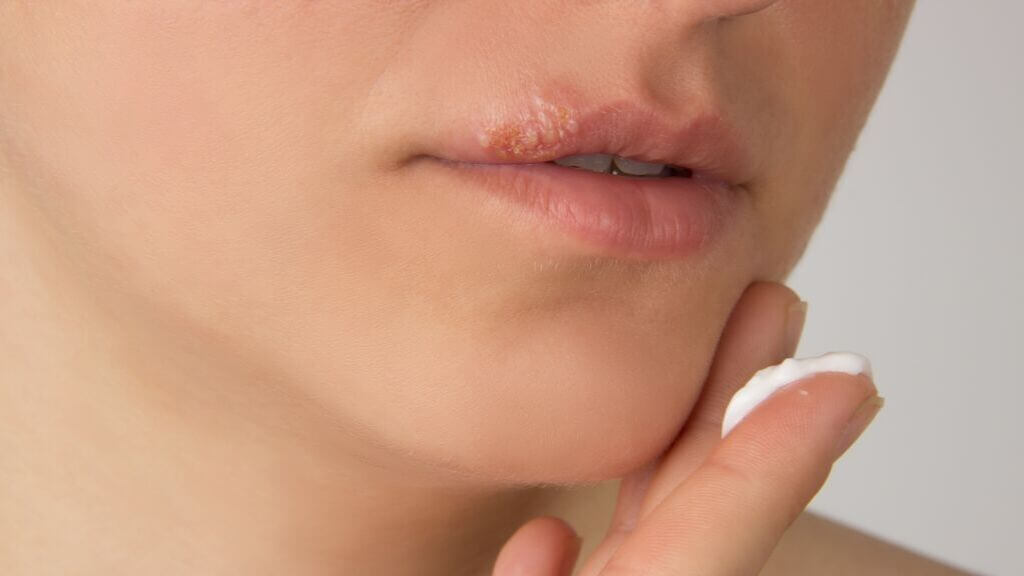
Once exposed to the virus, you can develop cold sores and mouth inflammation through your adult life. It is common for a fever to accompany this infection, and blisters will appear a few days after the fever shows.
The infection will typically last close to ten days. This condition can be treated with antiviral medications, and while it will not cure you, it is an effective way to shorten the duration of the cold sore.
Aphthous Stomatitis
This condition is also caused by a virus but is not contagious. It is caused instead by inadequate oral hygiene or damaged mucous membranes.
Canker sores are round with a red and inflamed border and a white center. The sores typically heal within two weeks, but larger sores can last for longer and can leave scarring.
Treatment is not required for this condition, but when larger blisters are present, you can apply topical creams to ease discomfort. Medications are only prescribed for larger breakouts.
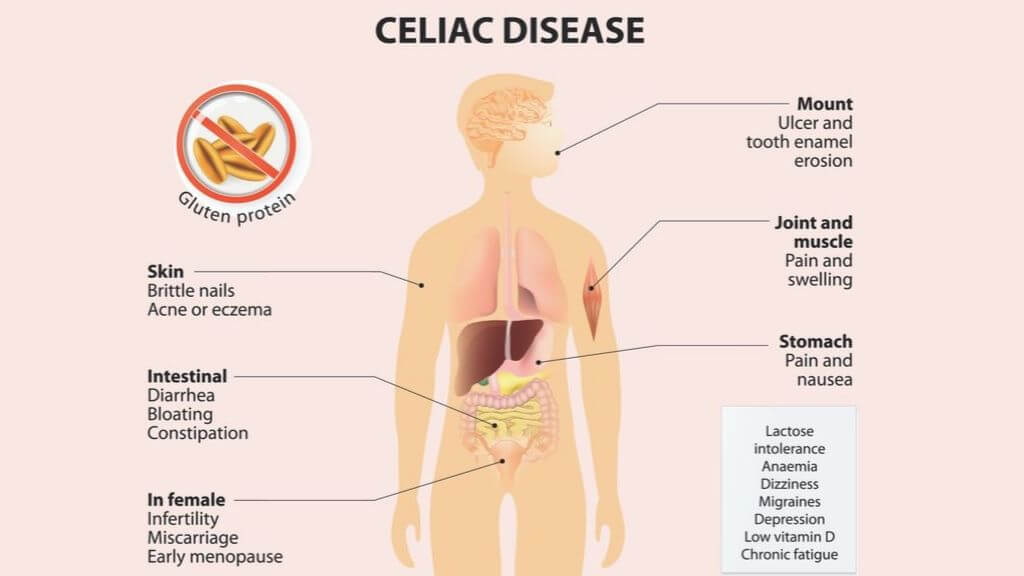
Additional medical conditions that are associated with mouth redness include:
♦ Celiac disease: This autoimmune disease is marked by an extreme immune response to gluten, the protein found in wheat. People with celiac disease are prone to mouth redness and oral ulcers, especially when exposed to gluten.
♦ Food sensitivities: As with gluten, any allergy or sensitivity to a food can cause a reaction within your mouth. Mouth redness, sores, and inflammation are common when eating a food you have an intolerance or sensitivity to.
♦ Allergic reaction to bacteria: People can be allergic to bacteria in the same way they can be allergic to foods, and if consumed, bacteria can cause a reaction in the mouth.
♦ Inflammatory bowel diseases: Stomach ulcers and mouth ulcers are common in those with inflammatory bowel diseases such as Crohn’s disease and ulcerative colitis. In many cases, mouth ulcers and mouth redness is the first sign that you are going to have an IBD flare.
♦ Autoimmune diseases: These diseases are marked by an overactive inflammatory response that attacks healthy cells and tissues. The widespread inflammation targets all parts of the body, including the mouth. Those with an autoimmune disease may notice mouth redness and soreness when the disease and inflammation are especially active.
♦ Lupus: Mouth ulcers and redness are the most common symptom of lupus. Unlike other mouth ulcers, those associated with lupus are situated on the roof of the mouth and not the gums or sides.
♦ Bechet’s disease: This disease causes inflammation of blood vessels and frequently causes mouth ulcers and soreness as a result of oral inflammation. You will notice a small round lesion to start, and it develops into a painful ulcer with surrounding redness to the tissue.
♦ HIV/AIDS: Mouth redness and ulcers are common for those with HIV/AIDS. As the infection progresses and the immune system weakens, mouth ulcers and sores become more frequent.
♦ Stress: Stress triggers the release of inflammatory chemicals that can cause the tissues in your mouth to become inflamed. During times of stress, it can be painful to eat, and you may notice redness, soreness, and even a swollen tongue, depending on the severity of the inflammation.
♦ Weakened immune system: A weak or suppressed immune system is unable to fight off invading pathogens, so bacterial infections are more likely. Since we are exposed to numerous bacteria through our foods, the mouth is a common area to experience an infection or bacterial overgrowth. A weakened immune system often accompanies mouth redness and sores.
♦ Candida Albicans infection: Candida Albicans is the most prominent fungal infection in humans, and it is characterized by a white coating in the mouth and on the tongue. The yeast is similar to oral thrush, and it can create white patches as well as inflammation and redness in the mouth. Antibiotics and probiotics can help to eliminate the harmful bacteria and promote the growth of the beneficial bacteria that work to keep Candida in check.

Prevention of Mouth Redness
Once you have the HSV-1 virus, you will have it for life, but you can take precautions so as not to pass it along. Do not share utensils or kiss anyone while you have an open sore.
As the most common cause for mouth redness and sores, the HSV-1 virus can be treated, but prevention lies in taking care not to pass along the contagious virus.
B vitamins are known to help prevent the development of canker sores along with proper oral hygiene. By eating more foods such as broccoli, spinach, lentils, and asparagus, or by taking B-vitamin supplements, you can prevent canker sores.
Take care of your teeth and avoid accidental trauma to the mouth, such as biting your cheeks or wearing dentures that do not fit properly.
Natural Treatment for Mouth Redness
There are a number of conditions that can cause mouth redness, but they have one common underlying connection. Inflammation is the root cause, but it is triggered by different infections or illnesses.
A weakened immune system, autoimmune conditions, allergies, and stress all trigger inflammation that can cause mouth redness. There are natural ways that you can reinforce the strength of your immune system, reducing your risk of mouth redness.
♦ Probiotics: Lactobacillus acidophilus supports gut health, which ultimately enhances immunity. This probiotic also helps with allergies that can trigger mouth redness. Lactobacillus rhamnosus is another beneficial probiotic that promotes immunity by keeping the gut bacteria in balance.
♦ Prebiotics: Prebiotics like NutraFlora prebiotic fiber do not treat inflammation directly, but they support the probiotics that do. This fiber is the perfect food source for probiotics, allowing them to flourish and prevent the colonization of harmful bacteria.
♦ L-lysine: This amino acid acts as an anti-inflammatory agent for your nervous system. By inhibiting viral loads, l-lysine reduces the number of vital neurotoxins in the body that can activate inflammation.
♦ Zinc: Zinc is an antioxidant and anti-inflammatory mineral. Studies have shown that zinc supplementation reduces the activation of inflammatory chemicals, which can reduce symptoms like mouth redness.
What Is the Long-Term Outlook?
Mouth redness and sores that are accompanied by additional symptoms or fever need prompt medical attention. Identifying the cause of the mouth redness is essential for effective treatment, and if the infection is contagious, take care not to spread it to others.

If a medical condition is the cause of your mouth redness, seek treatment for the condition, and your mouth will heal. Mouth redness can be effectively treated, so it is important to pay attention to symptoms.