Is it Osteoarthritis (OA) or Psoriatic Arthritis (PsA)? A Quick Guide
9 minute read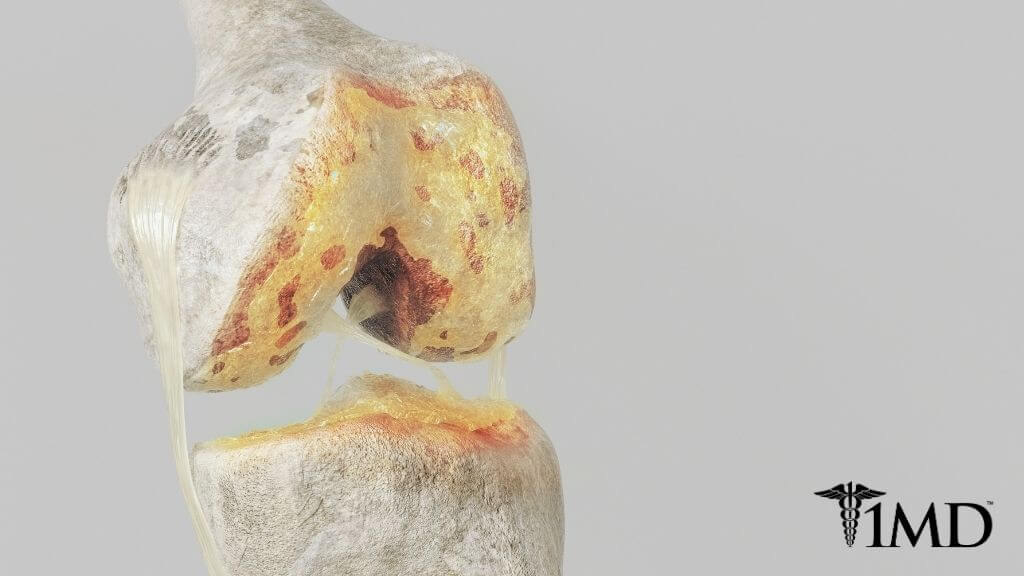
Most people have heard of arthritis and know that it’s a condition that affects joints, most commonly in older people. But there’s so much more to know and learn.
Did you know that there are at least 100 different types of arthritis and related conditions? Arthritis is not just an illness of the older population either. It can affect all ages, sexes and genders. But it’s true that it does typically occur in older women.
In addition to joint pain, arthritis refers to joint swelling, decreased range of motion, and stiffness. While the disease may come and go and vary in intensity, it is usually a progressive disease that can lead to permanent joint changes and visible physical changes. Some types of arthritis can also affect a person’s heart, eyes, lungs, kidneys, and skin.
Let’s look at a couple of types of arthritis that have been in the news a lot lately and how you can tell if you may have one or the other.
Osteoarthritis (OA)
Osteoarthritis is the most common type of arthritis, and it’s typically what people think of when they hear the term arthritis. When your cartilage wears away to the point at which bones are rubbing against one another, you develop side effects of this bone-on-bone action.
| Related: The Best Diet and Natural Treatments for Fighting Osteoporosis |
Generally, people seek relief for the joint discomfort, pain, swelling, and stiffness they feel in these areas. As time goes on, the joints are more affected and can become chronically bothersome and less strong and resilient. This is typically considered an age-related disease.

To that end, turmeric, boswellia serrata, and collagen are often used to help, finding a supplement containing bioavailable forms of these ingredients is a good idea.
Osteoarthritis Risk Factors
Are you wondering if you’re prone to osteoarthritis? The following osteoarthritis risk factors can help you determine if this is something that may play a role in your future healthcare regime.
| Related: How to Fight Osteoarthritis Flare Ups Naturally |
Family history: If you have family members who have osteoarthritis, then you may be genetically preprogrammed to have this condition.
Age: Because wear and tear play such a significant role in the development of this disease, it’s clear that the older you are the more likely you are to encounter osteoarthritis.
Gender: While women suffer from arthritis more often than men, osteoarthritis is a little more gender-neutral in its approach. It’s more common in men to develop the disease before age 45. After age 45 it’s more common for women to be diagnosed with osteoarthritis.
History of Injuries: If you have had an injury to a joint or the surrounding muscles and ligaments, you may be at greater risk of developing osteoarthritis down the road.
Obesity: Being overweight puts increased pressure and stress on your whole body, but your joints are particularly taxed, especially knee, hip, and spinal joints.

Repetitive Motion Occupations. People who have jobs that require them to make the same motions, day after day, all day long are at greater risk of osteoarthritis. This is simply because they’re overworking those areas.
| Related: How to Prevent & Identify Carpal Tunnel, Then Get Relief |
This risk factor extends beyond work and can also include sports and hobbies that require repetitive actions.
Poor Posture: The good news here is that you can work to correct your posture, but chronic bad posture habits put added stress on your joints.
Other Medical Conditions: If you have another health condition that can affect your joint health, then it’s important to discuss this and your chances of getting osteoarthritis with your healthcare provider. It’s better to be prepared than surprised by future complications.
Psoriatic Arthritis (PsA)
While osteoarthritis typically comes with age, overuse, and possibly an injury, psoriatic arthritis is very different. PsA is an autoimmune disease, which means that your body mistakenly attacks its own cells.
Almost all people who develop PsA have psoriasis, and the majority of them develop psoriasis first. This does not mean that if you have psoriasis you’re doomed to get PsA.
In fact, it’s estimated that of the 7.5 million people in the United States that have psoriasis, only about 20-30% of them have PsA.
Risk Factors for PsA
So, what are the risk factors for psoriatic arthritis? And remember, psoriasis is the largest predetermining factor for psoriatic arthritis. If you do not have psoriasis but are experiencing arthritic symptoms, you may want to ask your doctor if you possibly have osteoarthritis or another one of the many forms of arthritis.

| Related: Understanding Our Joints, Cartilage, and the Aging Process |
Age: Most people who develop PsA are between the ages of 30-50 but it can come on at any age.
Family History: Again, genetics plays a role in whether you’ll develop both psoriasis and/or PsA.
Psoriasis: As mentioned above, this is the leading indicator that the joint pain you are feeling is PsA. But don’t jump to any conclusions. Not all people with psoriasis develop PsA, and PsA symptoms may actually appear before psoriasis ones do, so the diagnosis of psoriasis may not have occurred by the time PsA crops up.
Types of PsA
There are five different types of psoriatic arthritis. They are divided and separated by what types of joints are involved. The types of PsA are:
Oligoarticular: This is when only four or fewer joints are affected. This is the most common type of PsA.
Polyarticular: Basically, the opposite of oligoarticular PsA, this type affects five or more joints.
Distal Interphalangeal (DIP): The joints of the fingertips are where PsA settles in this type of the disease.
Arthritis Mutilans: Arthritis mutilans is possibly the most debilitating and severe version of PsA, and it can destroy the small bones in the fingers.
Psoriatic Spondylitis: Here the spine is affected, and patients feel stiffness anywhere from their neck down to their low back region.
Treatments for Arthritis
The first step in finding the right treatment for your arthritic symptoms is determining which type of arthritis you have, if you have it at all.

The treatments for arthritis are varied. Plus, there are a whole host of new drugs and prescriptions that target different types of arthritis to give you the most effective treatment possible for your joint pain symptoms.
Once you and your doctor have made a diagnosis and are discussing your treatment plan, you may want to try some alternative treatments as well to bolster your pain relief and improve your quality of life.
Ask about the following alternative options to add to your healthcare regime.
♦ Acupuncture
♦ Massage
♦ Natural joint relief supplements, such as EasyFlex by 1MD
♦ Yoga and other forms of exercise
♦ Assistive devices to relieve pain/stress
The Bottom Line
The best part about seeking professional help and getting the right arthritis diagnosis is that you are now on your way to finding the best treatment and pain relief options for you.