Why Antibiotics Can Make Oral Infections Worse+Probiotics for Health
8 minute read
You can follow all the advice your dentist gives you and still be at risk for oral infections or disease. This is because most people do not realize that the use of antibiotics can have deleterious effects on our body’s natural defense against infection.
The friendly bacteria living within us can protect us against harmful pathogens, so the prescription of antibiotics may be important for your overall health, but some of their damaging aspects, such as worsening the risk of oral infections, need to be compensated for during treatment.
The Bad Side of Antibiotics
The presence of bacteria in our gut is no surprise. Trillions of bacteria live within us and help to support efficient digestion, immunity, and overall health.
| Related: How Probiotics Give Your Immune System a Big Boost |
These beneficial microorganisms work to take care of us so long as we take care of them. Unfortunately, we are prone to certain behaviors that are detrimental to these microscopic organisms, and we find ourselves needing to make necessary changes to support them.
It is not uncommon to be prescribed a course of antibiotics for an oral infection or any other infection. These drugs are designed to kill the bacteria causing the infection or illness.
As great as the development of these drugs was in the fight against disease, they come with one major flaw—antibiotics target and kill bacteria indiscriminately, which means they take out the good bacteria too.
Most research done thus far on the impact of antibiotics has not touched the realm of oral care. Recent studies of our friendly flora found that they produce beneficial fatty acids and impact white cells in a way that prevents oral infections.
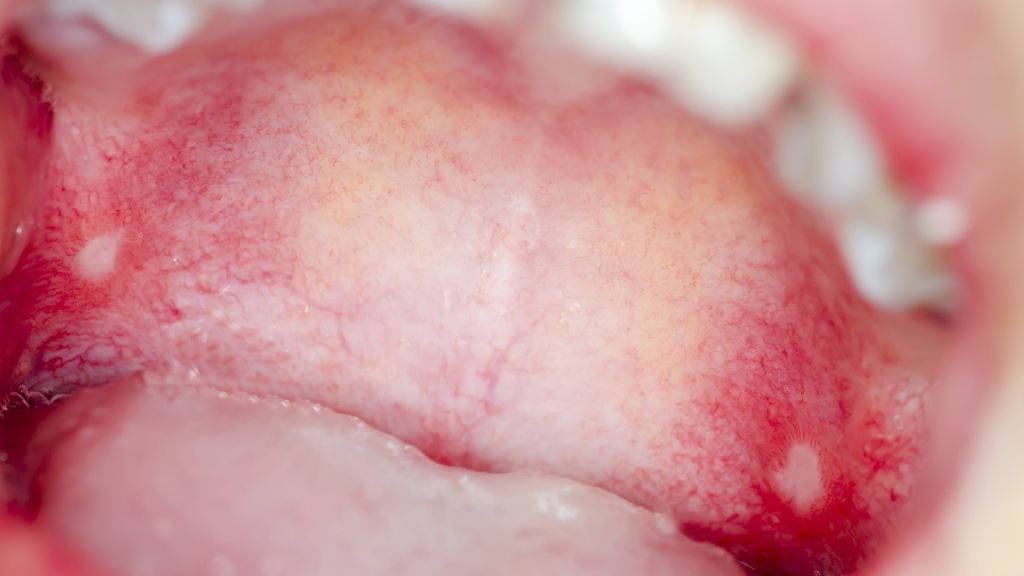
What this means is that taking antibiotics for an infection elsewhere in your body could kill bacteria protecting your mouth, leaving you at risk for an infection in your mouth as well as other areas on your body.
| Related: Fight Off Cold Sores With These Natural Immune Boosters |
The goal is to target a harmful bacterium and yet you damage a natural protection system instead. The good bacteria living within you naturally defend against inflammation and infection and antibiotics prevents this from happening. Not only does taking antibiotics result in reduced bacterial communities and health protection, but the beneficial fatty acids they produce, which regulate immune system responses are also depleted.
Supporting the Good Fight
Infections are a part of human existence. With so many potential toxins and pathogens in the world, infection and disease are simply inevitable.
| Related: New Vaccine Could Be Secret to Autoimmune Disease Prevention |
Thankfully, human evolution has developed natural defense mechanisms, including a host of friendly bacteria residing in your gut. While digestive benefits are an important role of these bacteria, they also provide support for heart health, mental health, and overall immunity.
As we have seen, the overuse of antibiotics contributes to the depletion of this friendly flora. There are also dietary and lifestyle choices we make that can cause the same problem.
The good news is that in the same way we can harm your gut microbiome, we can also protect and support optimal function. Here’s how:
Diversity in Your Diet
The more diversity you have in your diet, the healthier you and your gut bacteria will be. Optimal health and protection from infection depends on a diverse range of bacteria, which in turn depends on the diversity of your diet.
Specifically, you want to include plenty of fresh fruits and vegetables, as well as whole grains. The dietary fiber that gut microbes crave can be found in almost all plant-based foods.
| Related: Why Is Fiber Such an Important Part of Your Health |
Not only are these foods full of beneficial nutrients for you, but they support the strength and function of your microscopic defense system.
Cut Out Processed Foods and Sugars
Sadly, the typical Western diet contains high-fat, sugar-laden, processed foods. These foods are not only bad for your health, but they allow harmful bacteria in your gut to thrive.
If these should colonize in your gut, they push beneficial strains out and your risk for infection grows. It is best to stick with natural and fresh foods and avoid anything processed and full of sugar in order to maintain a healthy gut flora balance.
Prebiotics
Your gut bacteria require certain nutrients to grow and thrive. Prebiotics are food sources of dietary fiber that you cannot digest, but your friendly microbes can.

Regular inclusion of prebiotic foods in your diet provides gut bacteria the nutrients they need to thrive, and in return they produce the short-chain fatty acids that support your immunity.
Highly recommended prebiotic foods include bananas, asparagus, oats, leeks, onions, apples, lentils, and even dark chocolate.
Probiotics
Different from prebiotics, these are food sources or supplements that replenish and support existing gut bacterial communities. Because diet and use of antibiotics can deplete the bacteria numbers in your gut, regularly taking high-quality probiotics helps to maintain a healthy microbial balance.
Any imbalance in the gut environment can allow harmful bacteria to take over, which initiates inflammation and increases your risk for infection. Regularly taking probiotics not only supports your immune system, but it also boosts heart and brain health too.
Because the brain communicates with your stomach via the gut-brain axis, your mood and cognition is affected by the health of your gut as well.
Lifestyle Changes
Too much stress releases pro-inflammatory markers that inhibit the protective functions of gut bacteria. Inflammation is also linked to several serious diseases and is a key player in infections.

A lack of sleep contributes to increased stress and unbalanced gut microbial communities as well. To get the most from your friendly flora, be sure you get between 7 and 9 hours of restful sleep each night and reduce stress where you can.
Regular exercise has also been linked to increased numbers of beneficial bacteria in the gut.
The Bottom Line
Antibiotics are still very necessary, as they do give us advantages over serious illness and disease. However, the increased awareness of the benefits our friendly bacteria provide us allows us to rethink how often we prescribe and use antibiotics.
Our body is armed with natural defenses against disease, so we want to do our best to support this. We have to find a way to limit antibiotic use to only when necessary, so our natural protectors can do their part too.