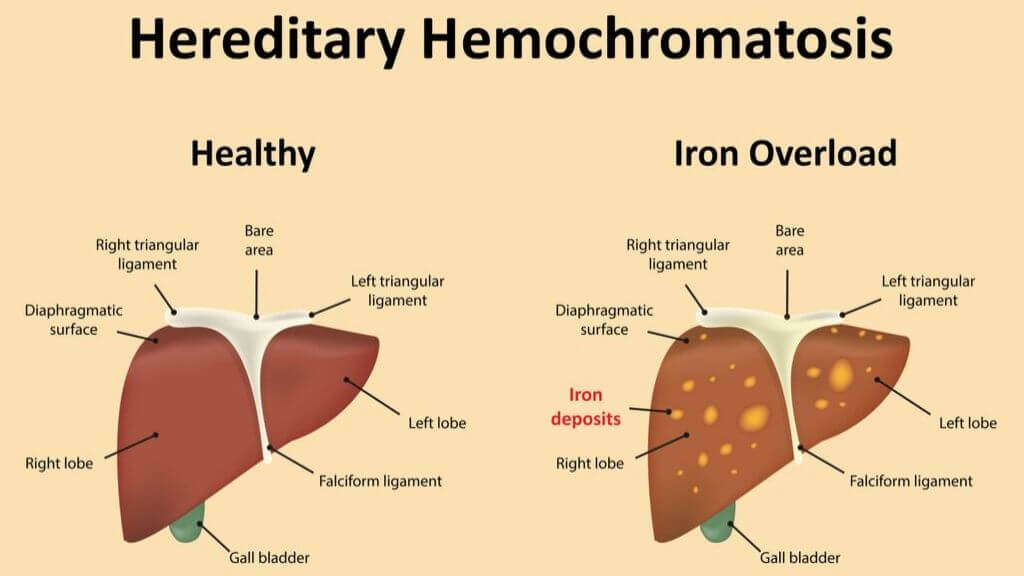
Hemochromatosis occurs when your body absorbs too much iron from the food you eat. This over absorption causes too much iron in your blood that your body is unable to get rid of. Iron that is deposited into your organs can cause oxidative stress and long term damage.
The most commonly affected organs are the heart, liver, and pancreas.
What Causes Hemochromatosis?
Hereditary hemochromatosis is caused by genetic mutations (primary hemochromatosis) of the HFE gene that controls iron absorption. You must inherit a mutated gene from each parent to develop this condition, but if each parent doesn’t carry it, you are only a carrier and will not show symptoms.
You can also develop hemochromatosis when iron builds up as a result of other medical conditions (secondary hemochromatosis). These conditions can include anemia, kidney dialysis, and chronic liver disease.
Hemochromatosis Symptoms
The early stages of hemochromatosis may not exhibit any symptoms. When they do appear, chronic fatigue is the first symptom, along with joint pain.
Pain in the knuckle (known as the “iron fist”), is often one of the first signs of the disease. Additional symptoms that may appear include:
♦ Abdominal pain
♦ Loss of body hair
♦ Loss of sex drive
♦ Heart flutters
♦ Lack of energy
♦ Memory or brain fog
♦ Weight loss
♦ Abnormal coloring of the skin (gray or bronze)
Hemochromatosis Diagnosis
Because symptoms of hemochromatosis can resemble those for other conditions, testing is the only way to accurately diagnose the condition.
Blood testing is done to measure the amount of iron-bound proteins in the blood, and DNA testing can be done to confirm the presence of the mutated HFE genes. You may also need a liver biopsy to test for liver damage, as the liver is the main storage place for excess iron and is the first organ to become damaged.
Hemochromatosis Treatment
The most common treatment is phlebotomy, which involves the removal of blood from your body. You need to get these done on a regular basis with hemochromatosis to continue moving excess iron.

Symptoms start to go away after phlebotomy treatment begins, but there are also some side effects that cause people to avoid this treatment. Fatigue and pain during the process are the most common complaints.
If you have a fear of needles or do not want to get phlebotomy, there are medications that can be used to treat hemochromatosis. These medications are more expensive and also have their own side effects, including pain at the injection site and flu-like symptoms. There is also medication that helps to expel excess iron in your urine and stool.
Hemochromatosis Diet
A hemochromatosis diet will limit your iron intake, and you should avoid iron supplements, raw seafood, and alcohol consumption. Raw seafood contains a bacterium known to proliferate in iron-rich environments, and this bacterium can cause serious health complications and death.
Alcohol causes serious damage to your liver, and the liver is the most sensitive to any excess iron in the body. Alcohol also causes enhanced absorption of iron from food, causing even higher levels of iron to accumulate in the liver.

Along with removing iron-rich foods from the diet, you also need to limit the intake of other nutrients that accelerate the absorption of iron.
Foods containing vitamin C and beta-carotene should also be limited. You do not want to avoid them completely, as they are essential to your overall health. You should eat foods containing vitamin C and beta-carotene separate to those containing iron, to get the nutrients you need without contributing to iron overload.
Natural Treatments for Hemochromatosis
Dietary modifications are the best approach to naturally reducing the symptoms of hemochromatosis. By limiting the amount of iron you consume, there is less chance of overload to your blood and organs.
In addition to this, there are some supplements that can help treat symptoms when used in conjunction with your doctor’s care plan.
♦ Turmeric: This ancient spice reduces iron absorption by safely binding and removing it from the body.
♦ Milk thistle: The compounds in milk thistle actively inhibit the absorption of iron.
♦ Calcium: This mineral can inhibit iron absorption, thus reducing the levels entering the blood from your food.

Antioxidants are also important, as oxidative damage is a fundamental problem associated with hemochromatosis. Antioxidants are found in most fresh fruits but are also available in supplements too.
Variations of Hemochromatosis
Four types of hereditary hemochromatosis are classified by the age of onset and the mode of inheritance.
♦ Type 1: This version affects men more than women and is caused by genetic mutations in the HFE gene. Symptoms develop by the age of 20.
♦ Type 2: This is also known as juvenile-onset hemochromatosis. This version results in an overload of iron in the blood and is caused by a mutation to the HFE2 and the HAMP genes.
♦ Type 3: This version is caused by genetic mutations to the TFR2 gene and occurs before the age of 30.
♦ Type 4: Also called ferroportin disease, this type of iron overload specifically impacts the heart, liver, and pancreas, and does not develop until adulthood.
Hemochromatosis Statistics
♦ Type 1 is the most common form of hemochromatosis in the United States and affects about 1 million people.
♦ If type 2 is left untreated, it can cause fatal heart disease by the age of 30.
♦ The onset of type 3 is generally before the age of 30.
♦ Approximately 10 percent of the Caucasian population is a carrier of classic hereditary hemochromatosis.

Hemochromatosis and Children
Hemochromatosis can also develop in children and is known as either juvenile or neonatal hemochromatosis. The juvenile version presents in a similar way to the adult form, and it affects children after the age of 15.
This type is always caused by a mutated HFE gene. Neonatal hemochromatosis occurs when iron builds up in the infant’s liver shortly after birth and sometimes can result in death.
What Is the Long-Term Outlook?
Hemochromatosis causes a progressive buildup of iron over time, and there is no cure. The most severe cases can lead to permanent scarring of the liver, which can cause liver cancer and liver failure. In these cases, the damage is also not reversible.
Early detection and diagnosis are essential to staying ahead of the condition. With treatment and dietary changes, you can prevent further damage and control the iron levels in your blood to better protect your health.