Type 1 and Type 2 Diabetes: The Differences You Need to Know About
7 minute read
Diabetes affects millions and yet much of the population remains confused about the different types of the condition. There are two types of diabetes, each with their own causes and each with their own impacts on the body.
Understanding the difference between them is important when it comes to diagnosis as well as treatment. Diabetes can be dangerous if not monitored and regulated, and knowledge is the first step to controlling the condition.
Understanding Diabetes
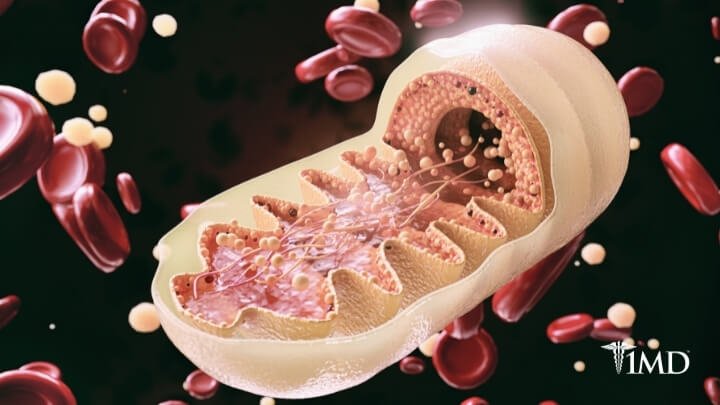
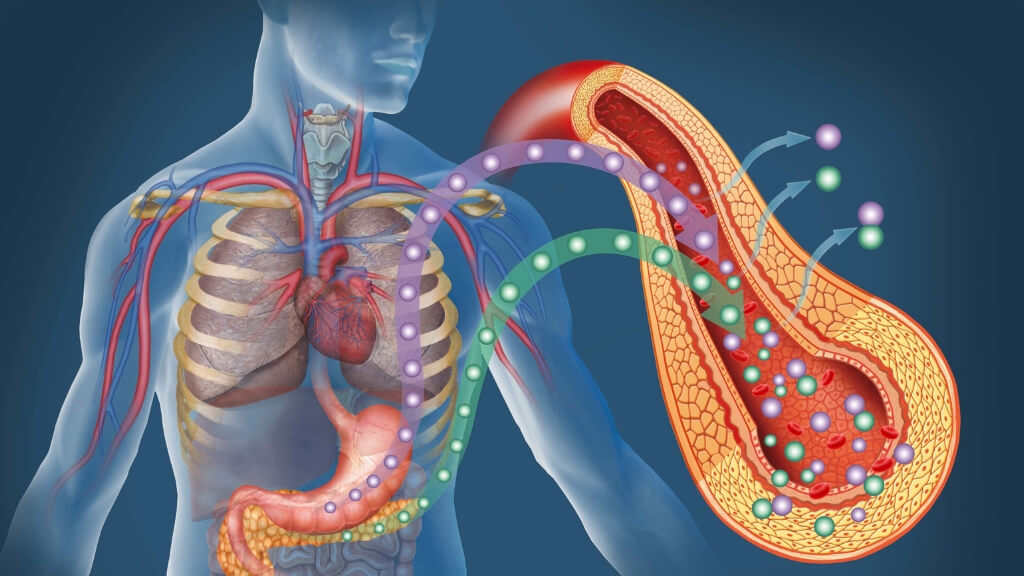
Type 1 and type 2 diabetes are both chronic conditions that impact the way your body regulates blood sugar (glucose). The difference between the two lies in the role of insulin. Glucose is fuel that our body needs to feed all your cells. Insulin is needed in order for this glucose to enter your cells.
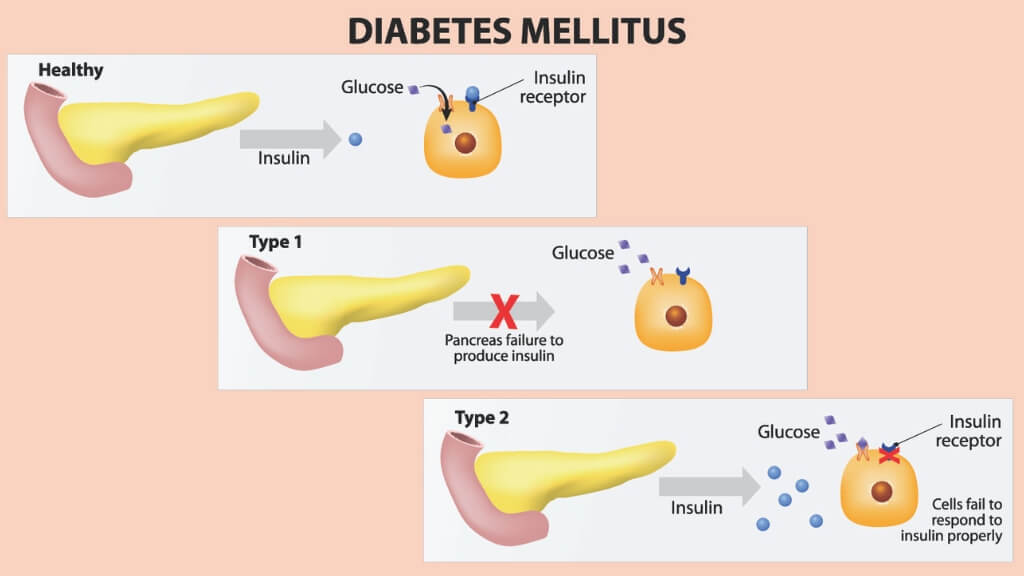
People with type 1 diabetes are unable to produce insulin, and those with type 2 do not respond to insulin the way they should.
Because uncontrolled diabetes can lead to very elevated levels of blood glucose and serious, possibly fatal, health complications, it is important to identify the disease early. The most common symptoms of diabetes include:

♦ Feeling thirsty all the time
♦ Frequent urination or feeling like you need to urinate
♦ Feeling hungry all the time
♦ Fatigue that is not resolved with rest
♦ Blurry vision
♦ Cuts or sores that take longer to heal than normal
♦ Irritability and mood swings (type 1 diabetes only)
♦ Tingling sensations or numbness in hands and feet (type 2 diabetes only)
Despite the similarity in symptoms, the two types of diabetes present very differently. Generally, people with type 2 diabetes will not notice symptoms for years, as they often develop slowly over time. Some people do not even notice any symptoms at all and the condition remains undiscovered until complications develop.
Type 1 diabetes develops fast and typically presents during childhood or adolescence.
What Causes Diabetes?
The two types of diabetes have very different causes, which is important when it comes to prevention. With type 1 diabetes, the immune system is involved, as it attacks your insulin-producing beta cells in the pancreas.
Your body has natural defenses against invading pathogens, but with type-1 diabetes the body mistakenly attacks healthy cells. Once they are destroyed, you are unable to produce the insulin you need.
With type-2 diabetes, your body produces insulin, but you develop insulin resistance. This means that your body is not able to effectively use the insulin, which impacts blood glucose levels. Your pancreas produces more insulin to compensate, but, because it cannot be used, blood glucose builds up in your blood.
Genetics can play a part in this type of diabetes, but other factors are known to contribute, such as physical inactivity, poor diet, and obesity.
Complications With Diabetes
Diabetes is commonly known to impact blood glucose levels, but many are unaware of the additional complications that can arise. Diabetes is also strongly associated with heart and liver diseases too.
High blood glucose levels that arise from either type of diabetes can damage the blood vessels that serve your heart. Damaged blood vessels are known to increase your risk for heart disease.
Studies have shown that individuals with diabetes are more likely to develop cardiovascular disease, and often this is the ultimate cause of early death.
The type of diabetes you have is not important when it comes to protecting your heart. What matters is treating and controlling the condition so as to minimize any possible cardiovascular damage. Following the right diet and controlling blood glucose levels is the best way to ensure this.
In addition to heart disease, diabetes is strongly linked to liver disease too. Both types of diabetes cause elevated levels of blood sugar and this sugar is stored in the liver. This increases your risk for nonalcoholic fatty liver disease, a condition where excess fat builds up around the liver.
| Related: The Complete Guide to the Fatty Liver Disease Diet |
Fatty liver disease can also contribute to the development of type-2 diabetes, so it becomes equally important to maintain liver health as a means to preventing diabetes.
What You Can Do
Because fatty liver disease can contribute to diabetes or make it worse, you can work to promote liver health as a way to prevent diabetes or prevent serious damage.
It is important to follow a balanced and nutritious diet in order to minimize fat and sugar consumption. Processed foods should be limited or avoided as these are known to contribute to sugar and fat storage in the body as well as obesity. You can also try nutritional supplements designed to help improve liver health.

If you are overweight, it is recommended to lose weight, as obesity increases your risk for both diabetes and fatty liver disease. With the two conditions strongly linked, weight control is a great way to prevent either from developing. Protecting your liver also involves limiting alcohol consumption, as too much alcohol can cause fatty liver disease as well as cirrhosis.
Reducing blood pressure and cholesterol will also help to protect your heart and liver and prevent or control diabetes.
If you have type 1 or type 2 diabetes, you should get regular checkups with your doctor regarding heart and liver health. Diabetes cannot be cured, so it is essential to maintain these checkups regularly to monitor any changes to liver and heart function.
The Bottom Line
Type 1 and type 2 diabetes are serious conditions, but early diagnosis and the right treatment can help minimize problems. Diabetes is serious with regards to the complications that can arise when it is not closely monitored.
Heart disease as well as liver problems can occur, so it is important to stay ahead of your diabetes. If you notice any symptoms reach out to your doctor, so you can start protecting your health before it is too late.