A wide variety of joints encompass the skeletal system, all of which are key physical points of connection between two bones. Your joints are responsible for both movement and the body's stability. As you age, these joints may begin to wear down, so understanding joint health is essential. Featured here are some questions to start you on the path to a greater understanding of joint health to keep you moving forward.
Joint function naturally declines with age as a result of wear and tear. Over one-third of adults over the age of 60 experience issues with joint mobility. As your joints age, they can become stiff and less flexible as cartilage deteriorates. Fluid can also accumulate in the joints, which increases swelling and further reduces mobility.
In a joint, bones do not directly touch but instead are cushioned by cartilage. This natural shock absorber deteriorates with age, causing the synovial membrane that keeps your joints healthy to thicken. This can lead to extra fluid accumulation in the joint, causing further swelling and discomfort. Additionally, ligaments may begin to shorten and lose flexibility, making joints feel stiff.
Many age-related changes to joints are caused by a lack of exercise. Being inactive causes the cartilage to shrink and stiffen, reducing joint mobility. Overusing a joint throughout your life can result in an even faster breakdown of cartilage. Trauma, injury, and poor posture may cause bones to become misaligned, providing additional causes of excessive wear on joint tissues.
Since bones are integral parts of every joint, many individuals with joint pain question whether there is a relationship between loss of bone density and joint deterioration. In that light, research has found that some immune-mediated joint conditions can be associated with a higher risk of bone loss.
Certain medications used to help relieve joint discomfort can have serious effects on bone health. Additionally, severe joint pain can lead to inactivity, which in turn contributes to bone density loss. Therefore, promoting joint and bone health together is the best way to maintain optimal mobility and flexibility.
Joints naturally wear down with use over time, but with the proper diet, exercise, and the right joint health supplements, you can maintain joint health longer. In addition to age, several factors that influence joint health.
♦ Gender: Estrogen plays a role in cartilage protection. Therefore, women have a greater risk of developing joint issues after menopause as estrogen levels decrease.
♦ Ethnicity: Certain ethnicities show a higher risk of developing joint issues, including African Americans, Hispanics, and Native American.
♦ Family history: Genetics plays a role in the increased risk of certain joint conditions.
♦ Smoking: Smoking is known to trigger immune system responses that can increase the risk of joint issues and aggravate existing conditions.
♦ Diet: Certain foods can aggravate joint discomfort by triggering immune responses. A poor diet may contribute to obesity, increasing stress on joints, leading to more rapid deterioration.
♦ Inactivity: A lack of regular physical activity weakens bones and muscles, which reduces joint flexibility and increases joint instability.
As joint tissues become worn, cartilage loss reduces cushioning within the joint, and bones may rub together. In addition to discomfort, several other complications may arise.
♦ Swelling
♦ Joint stiffness
♦ Immobility
♦ A sedentary lifestyle may lead to bone density loss (increased fracture risk)
♦ Infections
♦ Heart health complications
When you present with symptoms such as swelling, pain, stiffness, or immobility, your doctor will first conduct an interview and then a physical exam of the affected joint(s). The joint will be palpated and inspected both stationary and while moving, and range of motion will be tested. This will allow the doctor to identify the cause and severity of your abnormal joint function.
One of the most common range of motion tests performed is the active range of motion test, which looks at the individual's movement without assistance. Another option is the passive range of motion test, which looks at movement with the help of an outside source while the joint is relaxed.
In addition to looking at joint motion, specific blood tests may be utilized to identify more serious conditions. Measuring specific laboratory parameters may help to identify the etiology of joint discomfort due to an aberrant immune system response or possibly infection.
♦ RF (Rheumatoid Factor) and CCP (cyclic citrullinated peptide) antibodies: These tests look for highly specific antibodies associated with immune-mediated arthritis.
♦ Erythrocyte Sedimentation Rate (ESR) or C-reactive protein (CRP): An elevated ESR or CRP reading can be associated with joint stiffness and swelling.
♦ Antinuclear Antibody (ANA): This test looks for the presence of immune-mediated antinuclear antibodies in the blood.
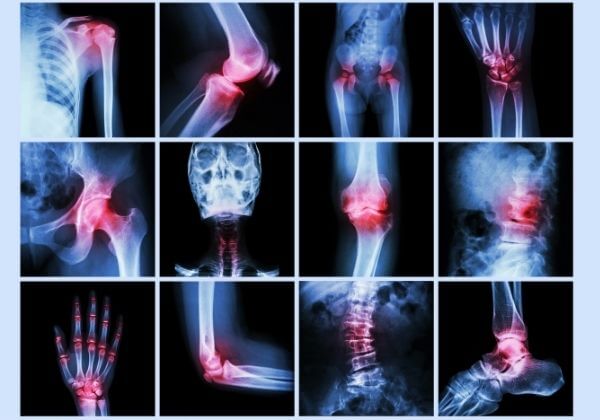
Your doctor will also evaluate the surrounding soft tissues, ligaments, and tendons. Imaging tests such as X-rays, MRI or CT scans, and ultrasounds can help identify abnormalities in joint structure. Additionally, nerve tests may be required if there is suspicion that nerves have become compressed by joint swelling or other nearby structures.
Treatment options are designed to alleviate discomfort and come in various modalities. Many of these include medications, such as oral or topical analgesics to help relieve discomfort. Minor joint issues can also be treated at home with ice therapy to reduce swelling or heat therapy to relax muscles surrounding the affected joint. Other treatment options may include:
♦ Physical therapy: A specific program designed by a physical therapist to help improve muscle strength to support and stabilize a weakened joint.
♦ Joint Injections: Corticosteroids can be injected directly into the affected joint to help reduce swelling and discomfort. As platelets stimulate the body’s ability to heal, platelet-rich plasma (PRP) injections may also be utilized.
♦ Bracing: Providing stability and compression around the joint using assistive devices can improve discomfort and mobility.
Surgery is typically reserved for situations where conservative treatment options have been unsuccessful. Should your doctor feel that surgery is necessary, the following may be recommended:
♦ Arthroscopic surgery, where the doctor can repair cartilage, menisci, and ligaments through small incisions.
♦ Joint resurfacing to repair cartilage defects in the joint.
♦ Fusion of two bones together in joints using pins, rods, or plates.
♦ Total or partial joint replacement involves removing a joint and replacing it with an implant that mimics a real joint's movement and function.
♦ Omega-3 fatty acids are powerful antioxidant compounds known to protect joint tissues in several ways. These contain healthy fats, which help to protect the joint from immune-mediated responses that can increase swelling and discomfort. Additionally, omega-3 fatty acids inhibit the production of specific proteins known to encourage fluid accumulation and swelling in joints.
♦ Maintaining a balanced diet with fresh fruits and vegetables, lean protein, healthy fats, and whole grains is best for joint health. Limiting or cutting out processed foods, high-fat foods, and alcohol also supports joint health by limiting the risk of immune responses that can cause joint discomfort.
♦ Regular physical activity is a great way to support joint health. Regular movement, stretching, and strength training can promote stronger, healthier joints and improve flexibility and mobility. By helping with weight loss, regular exercise can reduce the stress placed on your joints.
♦ Lifestyle changes are important in promoting better joint health. As mentioned, smoking is linked to an increased risk of joint problems, so quitting is a good place to start promoting joint health. You can also make minor changes to your daily routine to help support a more active lifestyle, such as taking the stairs instead of the elevator and parking further away from your destination so you can walk more.
It may seem that exercising will be difficult, but the opposite may actually be true. Regular low-impact exercise supports healthy joint function and also strengthens muscles, balance, and coordination. Individuals that live a sedentary lifestyle are prone to muscle atrophy, joint complications, and immobility. Physical activity can reduce the risk of age-related changes to joints and may even slow joint deterioration.
It is never too late to start living an active lifestyle.
♦ Resistance exercises such as lifting weights are beneficial for strengthening joints and muscles.
♦ Swimming and cycling are good for muscle health to help improve balance and joint stability.
♦ Tai Chi provides gentle movement of the joints to promote strength, balance, and stability.
♦ Daily stretches help to maintain joint flexibility and promote overall mobility.

Clinical research has identified natural ingredients that can support joint health and improve mobility. The natural ingredients in the physician-formulated supplement, MoveMD®️, support joint function and may even help slow the progression of joint deterioration.
♦ Boswellia serrata supports joint mobility by interfering with the chemical processes that contribute to the breakdown of cartilage. As a result, discomfort and swelling are reduced, allowing for smoother movement of the joint.
♦ Astaxanthin is a powerful antioxidant that has been clinically proven to outperform glucosamine and chondroitin. It helps alleviate joint discomfort, protects cartilage integrity, and promotes proper joint function and mobility.
♦ Both type X.I.V. eggshell membrane collagen and Type II chicken collagen combine to protect cartilage tissue and increase the range of joint motion and mobility.
♦ Hyaluronic acid helps promote joint mobility and flexibility by restoring synovial joint fluid, which reduces discomfort.
1MD Nutrition™ additionally offers CurcuminMD® Plus, which contains the new Longvida® Optimized Curcumin formula. This powerful ingredient has an absorption rate 285 times more efficient than standard curcumin, and it is this potency that protects both tissues and joints. Combined with the highly bioavailable form of standardized 65% Boswellia serrata, this curcumin supplement helps prevent cartilage loss to promote overall joint health.
KrillMD™ also promotes joint health with pure, Antarctic krill oil. More effective than fish oil, this krill supplement provides potent omega-3 fatty acids, delivered by phospholipids for more efficient absorption. KrillMD™ also contains astaxanthin, another potent antioxidant that helps support healthy joint function.
Cartilage in your joints gradually wears down over time, reducing shock absorption, mobility, flexibility, and in many cases, quality of life. Some joint conditions can be debilitating, but with a targeted approach, you can maintain healthy joint function.
A daily routine consisting of a balanced diet, regular exercise, and dietary supplement support can help you care for your aging joints. The revolutionary joint health formula, MoveMD®, targets joint function from the inside with clinically proven ingredients to support healthy joint function, alleviate discomfort, and promote mobility.
Dr. Adam Kreitenberg
Dr. Adam Kreitenberg is dual board-certified in both rheumatology and internal medicine. He completed his internal medicine internship, residency, and rheumatology fellowship at the University of Southern California and Los Angeles County Medical Center.